Can Aging Research Prevent the Next Pandemic?

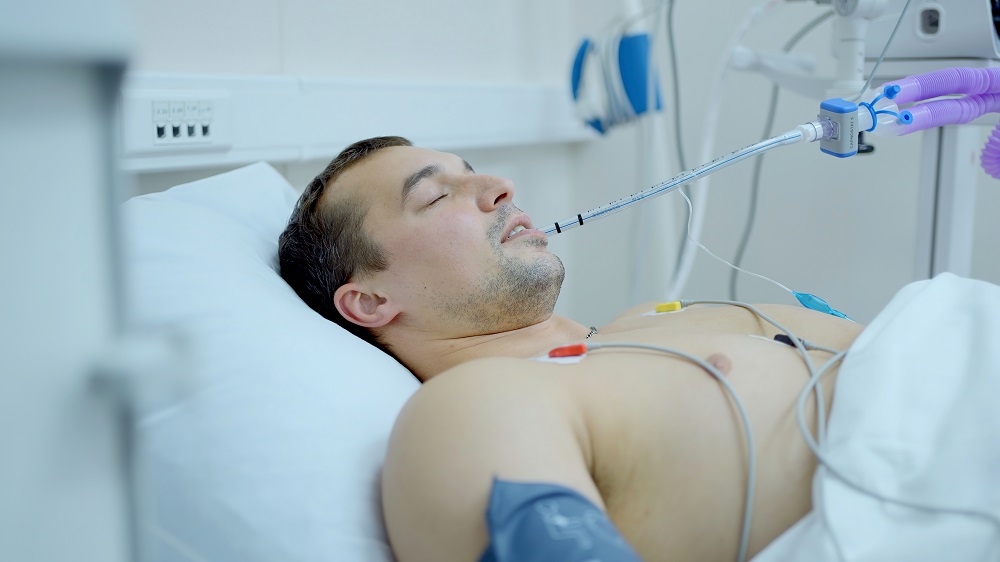
The world is reeling from the SARS-CoV-2 (COVID-19) pandemic, which has both had severe economic and humanitarian effects. As we continue to practice social distancing, we should ask ourselves: How can we avoid similar pandemics in the future?
Aging and infectious disease are linked
As we have discussed previously, aging is a major contributor to COVID-19 mortality rates. As this graph shows, your risk of dying to COVID-19 increases exponentially with age. It rises from 0.2% at the age of 20 to 8% at the age of 70 – an increase of 40 times!
This age-related mortality risk is not unique to COVID-19; other infectious diseases, such as the flu [1], also show an increase in their mortality rates as aging progresses. In addition to an increased mortality risk upon infection, the elderly are more likely to be infected by – and thus spread – pathogens, as has been shown with tuberculosis [2]. Because of this, it could be argued that any efforts to protect the elderly population could also protect the rest of the population, including the very young, from infection, which could arguably have effects that include the reduction of infant mortality.
These effects would work through herd immunity in the same way that a vaccine does. In fact, some therapies that work to reverse aspects of aging could improve the effectiveness of vaccines. This is because the immune system is weakened as we age, and this weakened immune system has a weaker response to vaccination [3]
The aged immune system is weaker because aging influences the immune system in multiple ways.
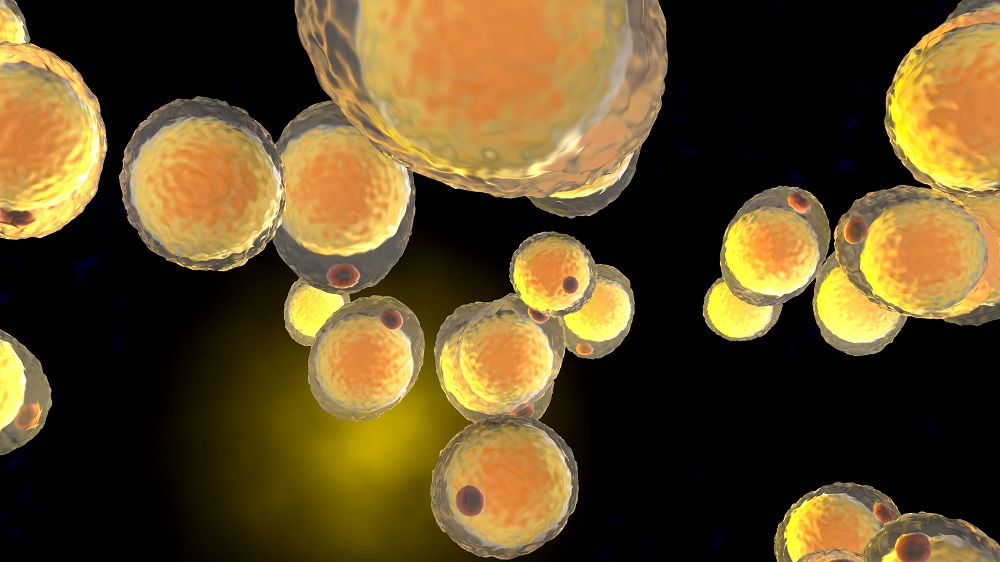
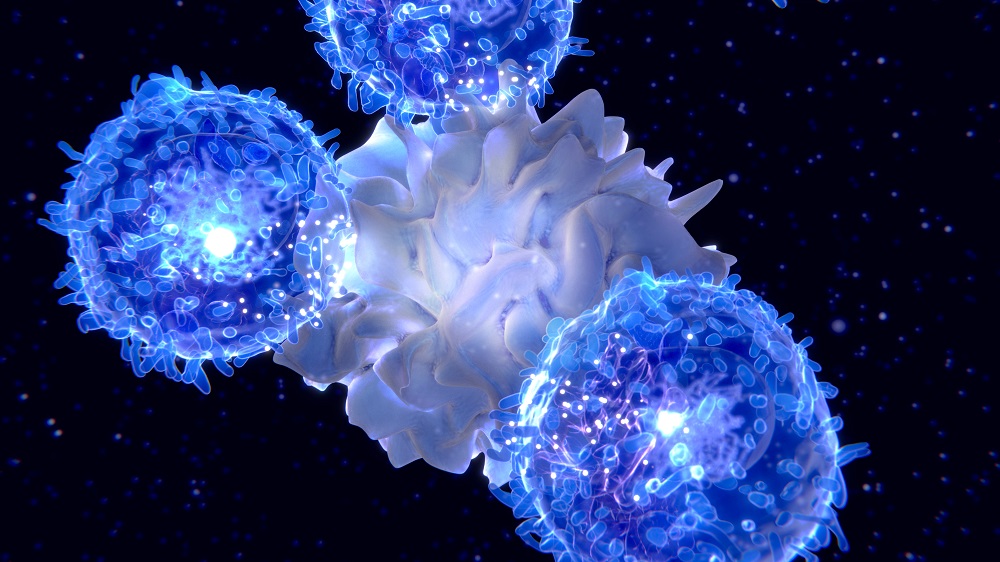
An important part of the immune system is its ability to respond directly to specific viruses or bacteria that infect us, which is why we can gain immunity to a pathogen after catching it and why vaccinations work. These specific responses rely, in part, on a particular type of immune cell – a ‘helper T cell’ – recognizing the pathogen and telling the rest of the immune system what antibodies are needed to kill it [4]. As we age, the ‘factory’ that matures these cells, the thymus, turns to fat and stops functioning in a process called involution [5], while the stem cells that contribute to the creation of these cells decrease their activity [6].
To make things worse, senescent cells, popularly known as zombie cells, build up in the tissues of the body as aging progresses [7]. These cells release a mixture of chemicals into the body that both cause inflammation and inhibit parts of the immune system [8], particularly the parts that are most harmed through the above changes.
It isn’t all bad news, though! While damage caused by aging does cause parts of the immune system to fall apart, scientists are rising to the challenge and developing drugs which may reverse this damage and restore the immune system. It’s still too early to be certain, but many of these scientists are now testing their drugs in humans, meaning that they may only be a few short years from the clinic if their trials are successful. lifespan.io has created the Rejuvenation Roadmap, a project that tracks the progress of aging research.
Rejuvenating the thymus
One of the most advanced efforts in this area is the effort to restore the thymus. Right now, two companies are trying to do this:
Repair Biotechnologies is trying to regenerate the thymus by activating a protein called FOXN1, which has successfully been used to regenerate the thymi of mice in other experiments [9]. Though the functional benefits of this approach in human infection are unknown, its research is promising, though it is focused on animals at the moment.
Intervene Immune is similarly trying to regenerate the thymus but is attempting to do so by injecting human growth hormone into patients [10]. Human growth hormone is known to have serious side effects, including increased risk of some forms of cancer [11]. Intervene Immune intends to reduce these side effects by injecting its patients with a range of other drugs, and – at least relative to the scale of its first human trial – it seems to have been successful in preventing the serious side effects previously seen in response to human growth hormone injection. It made headlines when treatment with its drug cocktail actually reversed markers of biological aging in humans [12] and may fully prove the effectiveness and safety of its therapy after two more human trials.
Between these two companies, Intervene Immune is the only one running human trials and is currently offering its therapeutic to the public through its website. However, the jury is still out on how effective or safe its therapy truly is, so it may be worth waiting a few more years to make sure it actually does have benefits without serious risks.
Other approaches are in the works
Some scientists are even starting to discuss the possibility of increasing the number of functional immune cells by destroying senescent immune cells [13]. Some immune cells deactivate themselves through negative feedback loops [14], so the hope is that the destruction of senescent versions of these cells could allow the remaining cells to activate and replicate, restoring active immune cell numbers. However, this has only been considered recently, and there has been very little progress in this area.
Other groups, such as the Lynne Cox lab, are looking at the possibility of inhibiting the inflammatory [15] and immunosuppressive [16] secretions of senescent cells in order to help restore immune functionality to a younger state. This research is still at an early stage, though it could have broad positive effects. It is certainly an approach that we will keep a close eye on!
Although this is promising, it is important to remember that there have been failures in the past. ResTORbio recently attempted to use a drug that inhibited mTOR (and thus improved the housekeeping function of autophagy in cells [17]) to restore immune function. Although initial human results were promising, a larger-scale study that we reported on previously found the drug to have no significant positive effects. This goes to show that, while optimism is warranted in some cases, it should be tempered with the knowledge that, in science, nothing is certain.
Conclusion
In the end, beyond its more obvious results, aging can contribute to death from, and infection by, multiple types of pathogens. Much like vaccination provides herd immunity and reduced symptoms from a particular disease, therapeutics to restore the aged immune system may provide a level of herd immunity against a wide range of diseases, increase the effectiveness of many drugs and vaccines, and even reduce the annual death toll from infections such as the common cold, which are mild in the young but deadly in the elderly. Hopefully, by the end of the 2020s, we will see the first of these therapies commercially available in clinics, though this is not a certainty, and which will succeed and which will fail are currently unknown. Still, there is reason for optimism and hope that rejuvenation therapies will stop the next pandemic from killing anywhere near as many people as COVID-19 has.
Literature
[1] Cromer, D., van Hoek, A. J., Jit, M., Edmunds, W. J., Fleming, D., & Miller, E. (2014). The burden of influenza in England by age and clinical risk group: a statistical analysis to inform vaccine policy. Journal of Infection, 68(4), 363-371.
[2] Thomas, T. Y., & Rajagopalan, S. (2001). Tuberculosis and aging: a global health problem. Clinical infectious diseases, 33(7), 1034-1039.
[3] Grubeck-Loebenstein, B., Della Bella, S., Iorio, A. M., Michel, J. P., Pawelec, G., & Solana, R. (2009). Immunosenescence and vaccine failure in the elderly. Aging clinical and experimental research, 21(3), 201-209.
[4] Janeway Jr, C. A., Travers, P., Walport, M., & Shlomchik, M. J. (2001). B-cell activation by armed helper T cells. In Immunobiology: The Immune System in Health and Disease. 5th edition. Garland Science.
[5] Dixit, V. D. (2010). Thymic fatness and approaches to enhance thymopoietic fitness in aging. Current opinion in immunology, 22(4), 521-528.
[6] Kim, M. J., Kim, M. H., Kim, S. A., & Chang, J. S. (2008). Age-related deterioration of hematopoietic stem cells. International journal of stem cells, 1(1), 55.
[7] López-Otín, C., Blasco, M. A., Partridge, L., Serrano, M., & Kroemer, G. (2013). The hallmarks of aging. Cell, 153(6), 1194-1217.
[8] Saleh, T., Tyutynuk-Massey, L., Cudjoe Jr, E. K., Idowu, M. O., Landry, J. W., & Gewirtz, D. A. (2018). Non-cell autonomous effects of the senescence-associated secretory phenotype in cancer therapy. Frontiers in oncology, 8, 164.
[9] Bredenkamp, N., Nowell, C. S., & Blackburn, C. C. (2014). Regeneration of the aged thymus by a single transcription factor. Development, 141(8), 1627-1637.
[10] Fahy, G. M., Brooke, R. T., Watson, J. P., Good, Z., Vasanawala, S. S., Maecker, H., … & Horvath, S. (2019). Reversal of epigenetic aging and immunosenescent trends in humans. Aging cell, 18(6), e13028.
[11] Swerdlow, A. J., Cooke, R., Beckers, D., Borgström, B., Butler, G., Carel, J. C., … & Ecosse, E. (2017). Cancer risks in patients treated with growth hormone in childhood: the SAGhE European Cohort Study. The Journal of Clinical Endocrinology & Metabolism, 102(5), 1661-1672.
[12] Fahy, G. M., Brooke, R. T., Watson, J. P., Good, Z., Vasanawala, S. S., Maecker, H., … & Horvath, S. (2019). Reversal of epigenetic aging and immunosenescent trends in humans. Aging cell, 18(6), e13028.
[13] Kasakovski, D., Xu, L., & Li, Y. (2018). T cell senescence and CAR-T cell exhaustion in hematological malignancies. Journal of hematology & oncology, 11(1), 91.
[14] Popmihajlov, Z., & Smith, K. A. (2008). Negative feedback regulation of T cells via interleukin-2 and FOXP3 reciprocity. PloS one, 3(2).
[15] Alimbetov, D., Davis, T., Brook, A. J., Cox, L. S., Faragher, R. G., Nurgozhin, T., … & Kipling, D. (2016). Suppression of the senescence-associated secretory phenotype (SASP) in human fibroblasts using small molecule inhibitors of p38 MAP kinase and MK2. Biogerontology, 17(2), 305-315.
[16] Ruhland, M. K., Loza, A. J., Capietto, A. H., Luo, X., Knolhoff, B. L., Flanagan, K. C., … & Schaffer, A. (2016). Stromal senescence establishes an immunosuppressive microenvironment that drives tumorigenesis. Nature communications, 7(1), 1-18.
[17] Jung, C. H., Ro, S. H., Cao, J., Otto, N. M., & Kim, D. H. (2010). mTOR regulation of autophagy. FEBS letters, 584(7), 1287-1295.