Rejuvenation Roundup October 2025
The trick-or-treaters have all gone home as the leaves have fallen to the ground, but rejuvenation biotech attempts to prevent human beings from fading away. Here’s what’s been done to fight aging in October.
Team and activities
 Our Campaign for Public Longevity: Public trust is the breakthrough that unlocks all others. The field of longevity science has long needed better tools to measure public sentiment in order to understand what drives that trust, and how to build it.
Our Campaign for Public Longevity: Public trust is the breakthrough that unlocks all others. The field of longevity science has long needed better tools to measure public sentiment in order to understand what drives that trust, and how to build it.
Thanks to your support, the Public Longevity Group (PLG) campaign is more than halfway to its goal, but there’s still time to make an even greater impact. We’re extending the campaign by two more weeks, with the LRI Board of Directors matching all donations up to $25,000 to push us across the finish line. That means every dollar you give will be doubled to support the launch of the first data-driven sentiment analysis engine for longevity science.
Interviews
 Joe Betts-Lacroix on Retro Bio and Its Recent AI Advancement: Retro Biosciences was founded about five years ago by the tech entrepreneur Joe Betts-Lacroix with a $180 million investment from his friend Sam Altman, the CEO of OpenAI.
Joe Betts-Lacroix on Retro Bio and Its Recent AI Advancement: Retro Biosciences was founded about five years ago by the tech entrepreneur Joe Betts-Lacroix with a $180 million investment from his friend Sam Altman, the CEO of OpenAI.
Sam Sharifi on Fixing Our DNA: Behind the vision of Sam Sharifi, PhD and Matter Bio’s Chief Scientific Officer, stands some serious science. Matter Bio has matured into a company with a pipeline and a cash flow.
 Andrea Maier on Longevity Medicine for All: Dr. Andrea Maier, Oon Chiew Seng Professor in Medicine at the National University of Singapore, is a veteran geroscientist and one of the most familiar faces in the rising field of longevity medicine. Andrea has been working on bringing longevity medicine to the public.
Andrea Maier on Longevity Medicine for All: Dr. Andrea Maier, Oon Chiew Seng Professor in Medicine at the National University of Singapore, is a veteran geroscientist and one of the most familiar faces in the rising field of longevity medicine. Andrea has been working on bringing longevity medicine to the public.
Advocacy and Analysis
Meet ALSAE: Improving the Cultural Image of Longevity: To challenge cultural stereotypes and misconceptions about longevity, a new organization aims to engage people who create culture. Its list of “cultural ambassadors” includes Oscar- and Grammy-winning artists.
Research Roundup
 Cell Cycle Stage Impacts the Efficacy of Senotherapeutics: A recent study reported that the effectiveness of the senotherapeutic drug ABT-263 depends on the cell’s DNA content, which is based on the cell cycle phase at which the senescent cell was arrested.
Cell Cycle Stage Impacts the Efficacy of Senotherapeutics: A recent study reported that the effectiveness of the senotherapeutic drug ABT-263 depends on the cell’s DNA content, which is based on the cell cycle phase at which the senescent cell was arrested.
Partial Reprogramming Enhances Nerve Repair in Rats: In Advanced Science, a team of researchers has explained how partial cellular reprogramming through the OSKM factors restores nerve repair ability to older animals.
 Impact of Off-Label Low-Dose Rapamycin on Healthy Adults: A team of scientists has concluded that there is no sufficient evidence that low-dose rapamycin use can extend healthspan and lifespan in healthy humans.
Impact of Off-Label Low-Dose Rapamycin on Healthy Adults: A team of scientists has concluded that there is no sufficient evidence that low-dose rapamycin use can extend healthspan and lifespan in healthy humans.
A Public Website for Evaluating Potential Anti-Aging Drugs: Researchers publishing in the International Journal of Molecular Sciences have showcased their creation of PASS GERO, a public-facing application that allows researchers to evaluate potential anti-aging compounds.
 Nanoparticles Potently Reverse Alzheimer’s in Mice: Scientists have created polymersomes, a type of nanoparticle, that latch onto a master regulator of amyloid-beta clearance, diverting it towards a more efficient route.
Nanoparticles Potently Reverse Alzheimer’s in Mice: Scientists have created polymersomes, a type of nanoparticle, that latch onto a master regulator of amyloid-beta clearance, diverting it towards a more efficient route.
Researchers Identify Key Age-Related Genes: In Aging Cell, researchers have described core genes that apply to a wide variety of species and appear to be causal drivers of aging.
 Why Naked Mole Rats Have Better DNA Repair: Scientists have found that the cGAS protein in naked mole rats, a famously long-lived species, boosts DNA repair, while the human version tends to hamper it. The difference boils down to just four amino acids.
Why Naked Mole Rats Have Better DNA Repair: Scientists have found that the cGAS protein in naked mole rats, a famously long-lived species, boosts DNA repair, while the human version tends to hamper it. The difference boils down to just four amino acids.
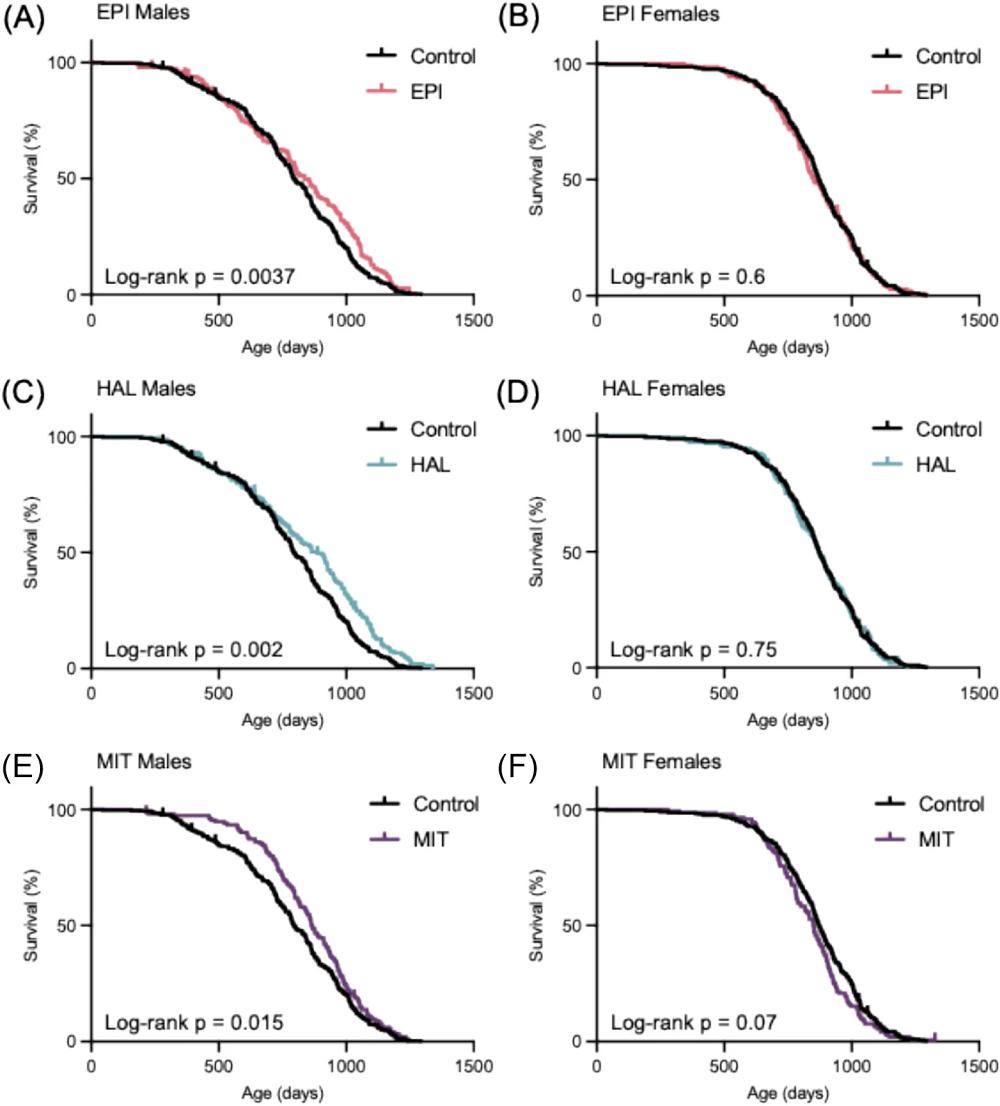
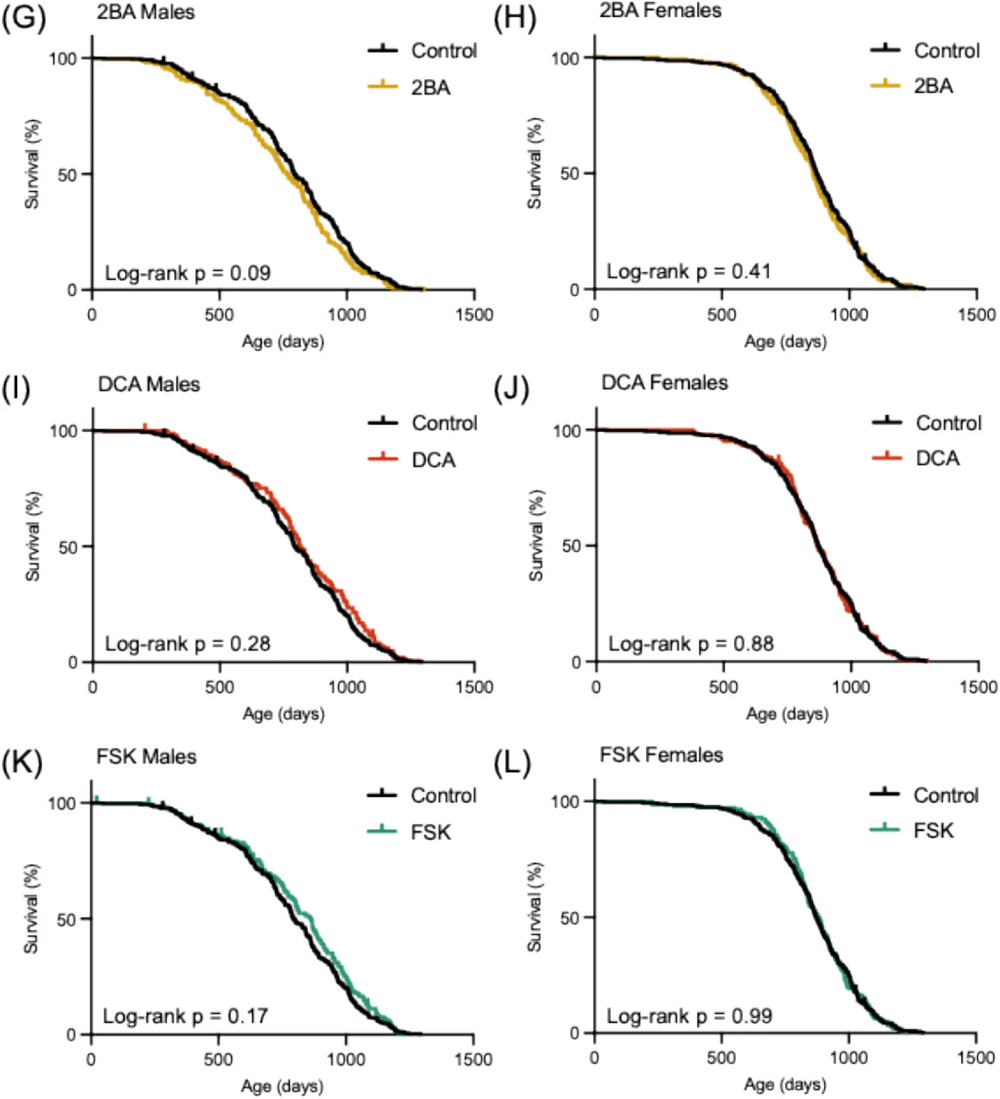
Interventions Testing Program Finds Three New Compounds: A new report from the Interventions Testing Program adds three new compounds to the list of lifespan-extending compounds confirmed during their experiments: epicatechin, halofuginone, and mitoglitazone.
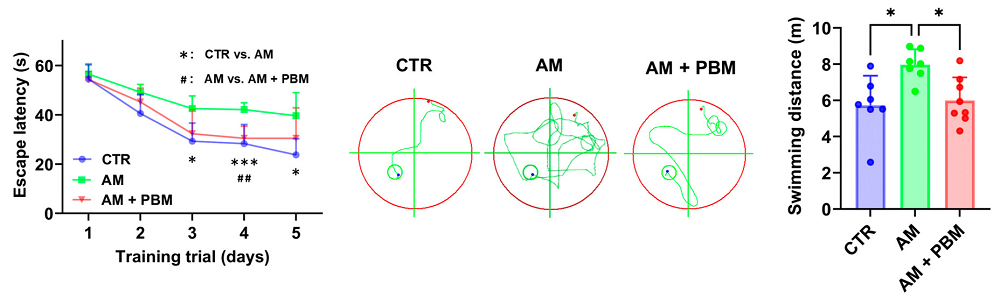
 Infrared Lasers Clear Harmful Compounds in Mouse Brains: Researchers have discovered that infrared lasers promote the clearance of toxic metabolites from the brains of age-accelerated mice by improving lymphatic drainage.
Infrared Lasers Clear Harmful Compounds in Mouse Brains: Researchers have discovered that infrared lasers promote the clearance of toxic metabolites from the brains of age-accelerated mice by improving lymphatic drainage.
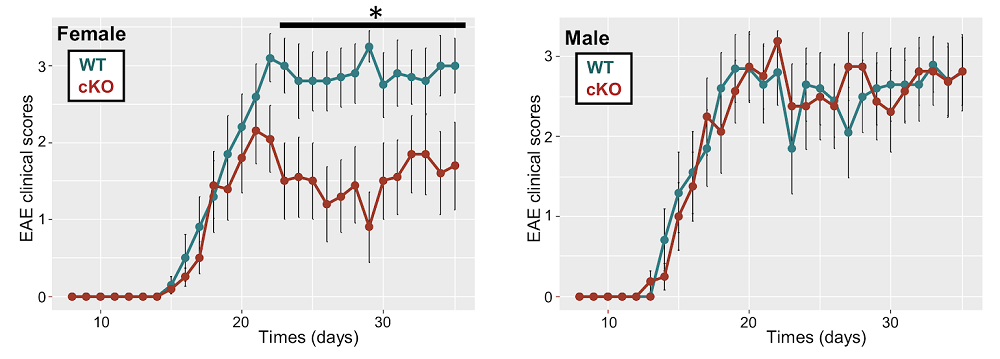
Female-Specific Mechanism of Neurodegeneration Discovered: Scientists have found that a gene on the X chromosome, which escapes silencing, promotes inflammation and neurodegeneration in a mouse model of multiple sclerosis, but the effects can be reversed with metformin.
 How Being in Orbit Affects Stem Cells: In Cell Stem Cell, researchers from the Cedars-Sinai Medical Center have published a review discussing what experiments conducted in space can do for stem cell research and medical research as a whole.
How Being in Orbit Affects Stem Cells: In Cell Stem Cell, researchers from the Cedars-Sinai Medical Center have published a review discussing what experiments conducted in space can do for stem cell research and medical research as a whole.
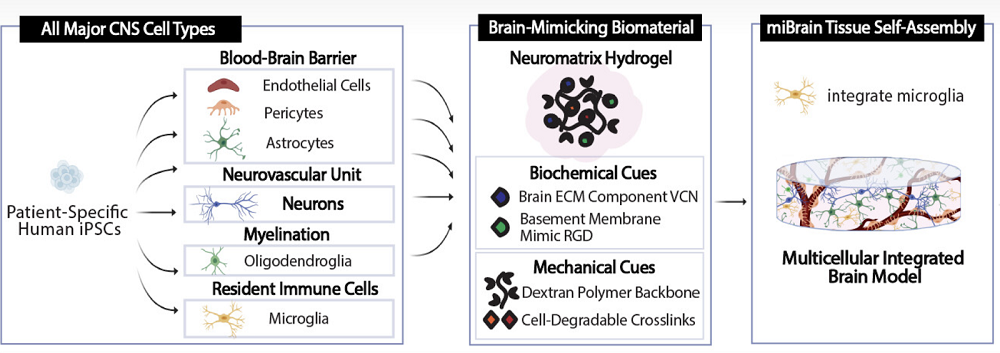
Tiny Brain Organoids Show Promise in Alzheimer’s Research: Scientists have developed a novel multicellular integrated brain model to study neurological diseases, incorporating all six major brain cell types derived from patient-specific induced pluripotent stem cells.
 Addressing Age-Related Vision Decline With Lipid Supplements: Researchers have partially reversed age-related vision decline in mice by injecting lipids directly into the retina.
Addressing Age-Related Vision Decline With Lipid Supplements: Researchers have partially reversed age-related vision decline in mice by injecting lipids directly into the retina.
Measuring Dog Aging With Protein Metabolism: Researchers working with data from the Dog Aging Project have found that post-translationally modified amino acids, which are generated from protein metabolism, are useful in determining the biological ages of dogs.
 Amyloid-Fibrinogen Complexes Exacerbate Alzheimer’s in Mice: A study from Rockefeller University suggests that an unholy duo of two proteins causes harm in much lower concentrations than either of them alone.
Amyloid-Fibrinogen Complexes Exacerbate Alzheimer’s in Mice: A study from Rockefeller University suggests that an unholy duo of two proteins causes harm in much lower concentrations than either of them alone.
Stiff Collagen May Lead to Senescent Cells: A preprint study has found that the stiffness of the extracellular matrix encourages cells to undergo senescence. These researchers placed cells into a hydrogel scaffold that can have its stiffness changed on the fly.
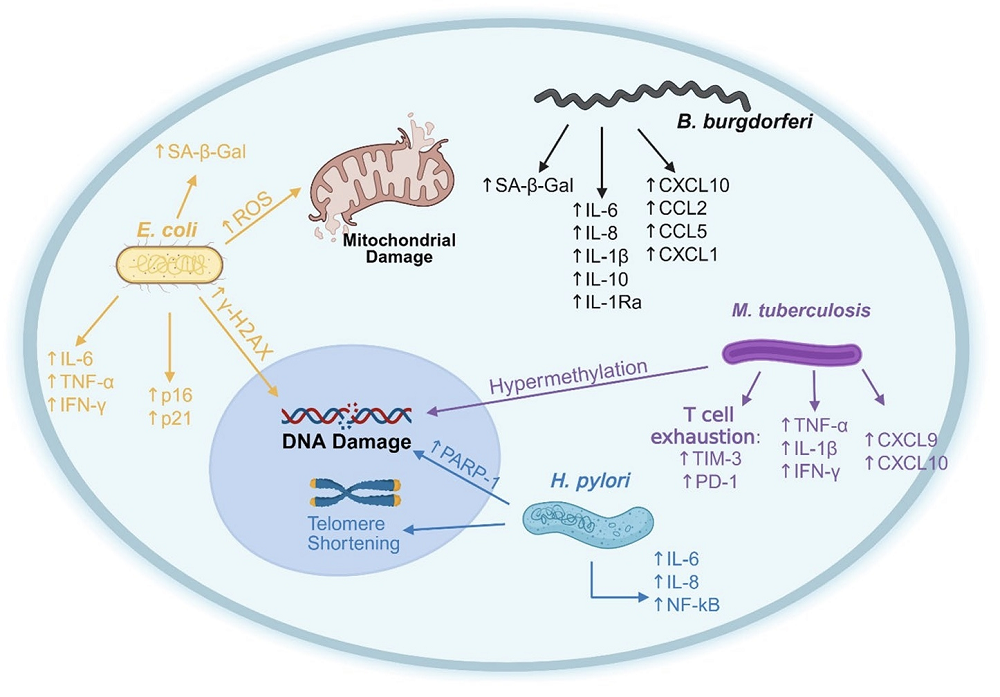
 Review Links Lingering Infections to Senescence: In a comprehensive review, scientists discuss the various mechanisms by which chronic infections drive cellular senescence and aging.
Review Links Lingering Infections to Senescence: In a comprehensive review, scientists discuss the various mechanisms by which chronic infections drive cellular senescence and aging.
Organ Fat Is Associated With Carotid Atherosclerosis: A recent study discovered an association between visceral and, to a lesser extent, hepatic fat with cardiovascular risk factors and carotid atherosclerosis.
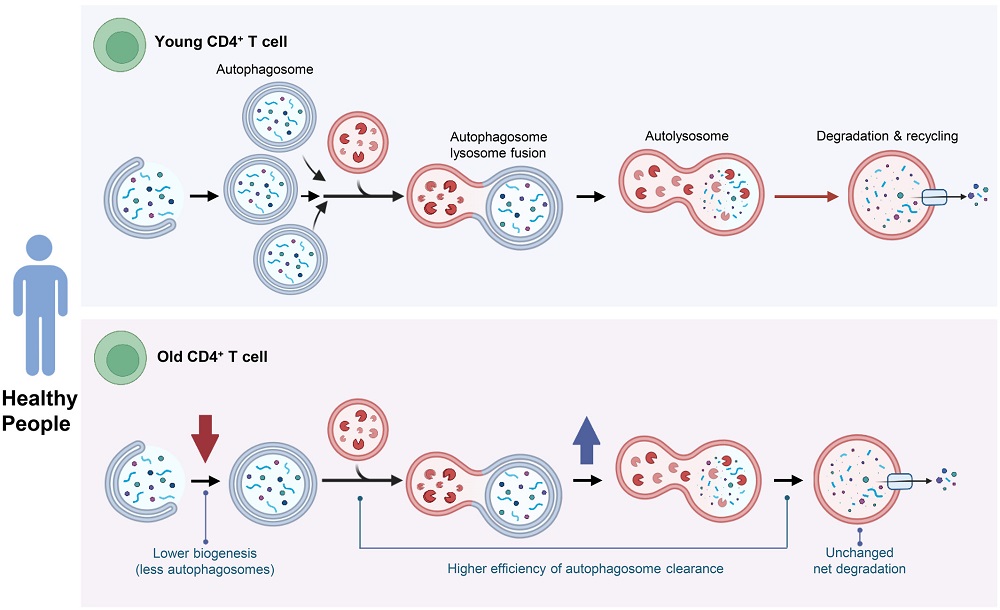
 Maintenance Stays Efficient in Healthy Older People’s Cells: Researchers publishing in Aging Cell have found that the efficiency of autophagy, a cellular maintenance process, increases rather than decreases in some T cells derived from healthy older people.
Maintenance Stays Efficient in Healthy Older People’s Cells: Researchers publishing in Aging Cell have found that the efficiency of autophagy, a cellular maintenance process, increases rather than decreases in some T cells derived from healthy older people.
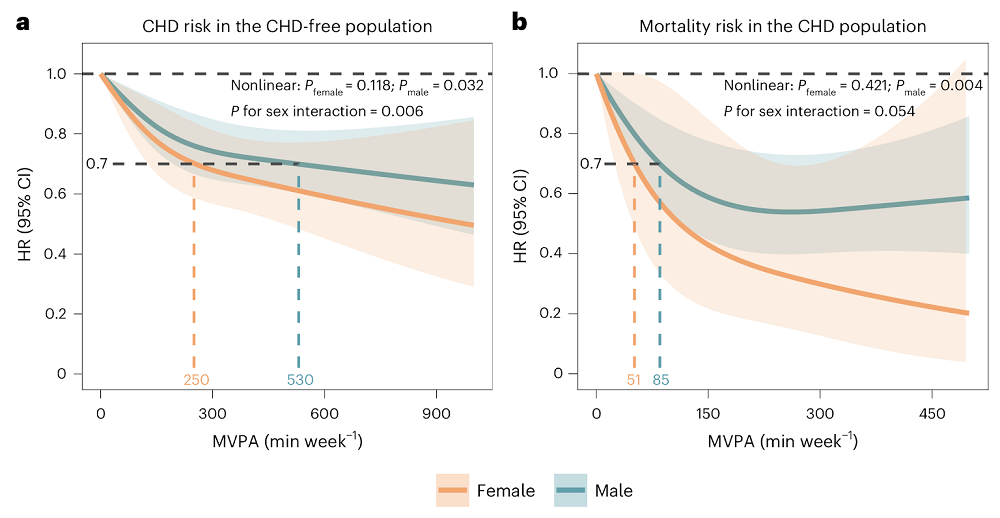
Men Might Need More Exercise to Lower Cardiovascular Risks: A new observational study suggests that men need more than twice as much exercise as women do to achieve the same level of reduction in the risk of cardiovascular heart disease.
Relationship between weekends catch-up sleep and risk of aging: Stratifying by bedtime, the relationship between catch-up sleep and reduced aging risk is only observed in individuals who usually go to sleep before midnight and have catch-up seep less than 2 hours.
Dose-response relationship of resistance training and the effects on circulating biomarkers of inflammation or neuroplasticity in older adults: These findings demonstrate that resistance training can significantly improve circulating biomarkers of neuroplasticity and inflammation and highlight key dose-response relationships critical for optimizing such programs.
An Ad Libitum-Fed Diet That Matches the Beneficial Lifespan Effects of Caloric Restriction: Ad libitum-fed diets can be designed to replicate, and potentially enhance, the geroprotective benefits of caloric restriction, albeit via different mechanisms, potentially offering a more sustainable dietary approach to longevity extension.
α-Lipoic acid mitigates age-related cognitive decline by modulating PPARγ/NF-κB-mediated neuroinflammation: Administration demonstrated significant cognitive-enhancing effects, accompanied by suppression of both microgliosis and astrocytosis, as well as a reduction in pro-inflammatory cytokines in the hippocampus of aged mice.
Effects of lifetime supplementation with ubiquinol 10 on the lifespan and progression of aging in female C57BL/6 mice: Maximum lifespans and survival curves did not significantly differ between the ubiquinol 10 and control groups.
Enhanced Selenium Supplement Extends Lifespan and Delays Multi-Organs Aging by Regulating the Sik1 Pathway Through Maintaining Calcium Homeostasis: This systematic approach provides a solid theoretical foundation and clinical evidence for the application of nano-selenium in anti-aging research.
Glycation-lowering compounds inhibit ghrelin signaling to reduce food intake, lower insulin resistance, and extend lifespan: As a late-life intervention, Gly-Low slows hypothalamic aging signatures, improves glucose homeostasis and motor coordination, and increases lifespan, suggesting its potential benefits in ameliorating age-associated decline.
Effect of the mitophagy inducer urolithin A on age-related immune decline: a randomized, placebo-controlled trial: These findings indicate that short-term urolithin A supplementation modulates human immune cell composition and function, supporting its potential to counteract age-related immune decline and inflammaging.
Combined creatine and HMB co-supplementation improves functional strength independent of muscle mass in physically active older adults: This combined approach represents a promising strategy for preserving functional capacity and promoting healthy ageing.
Pharmacokinetic analysis of intermittent rapamycin administration in early-stage Alzheimer’s Disease: These findings suggest that weekly rapamycin administration in Alzheimer’s patients results in acceptable pharmacokinetic variability, supporting fixed-dose regimens in future trials.
Mesenchymal stem cell derived extracellular vesicles reverses neural aging via OSKM modulation: This study represents a pioneering achievement in regenerative medicine, demonstrating the potential of microRNAs in extracellular vesicles to stimulate OSKM, a significant stride forward in addressing neural aging.
Dual-ligand engineered exosome regulates WNT signaling activation to promote liver repair and regeneration: Collectively, this work revealed the broad therapeutic effects of WNT signaling activation in the liver through the dual-ligand-carrying exosomes.
Effects of low-intensity pulsed ultrasound on muscle mass and Fndc5 mRNA expression in aged male mice: These findings suggest that this technique may serve as a safe, non-invasive intervention to counteract sarcopenia by promoting muscle growth and mitochondrial gene activation in aged skeletal muscle.
Effects of Computerized Cognitive Training on Vesicular Acetylcholine Transporter Levels in Healthy Older Adults: These findings clarify the neurochemical basis of cognitive training benefits, showing that speed training upregulates binding in networks that support attention, memory, and executive function.
The dissipation theory of aging: a quantitative analysis using a cellular aging map: These results provide a novel perspective on aging as a dissipative process and introduce a computational framework that enables measuring age-related changes with molecular resolution.
News Nuggets
 Agentic AI Against Aging Hackathon: HackAging.ai is the global online hackathon at the intersection of Agentic AI and longevity science, bringing together researchers, founders, and engineers to accelerate solutions that extend healthy human lifespan.
Agentic AI Against Aging Hackathon: HackAging.ai is the global online hackathon at the intersection of Agentic AI and longevity science, bringing together researchers, founders, and engineers to accelerate solutions that extend healthy human lifespan.
New Foundation Unites Hollywood and the Arts Against Aging: The Alliance for Longevity Science, Arts & Entertainment announced its official launch, pioneering a new nonprofit effort to accelerate progress against the chronic diseases of aging.
 NUS Medicine Launches New Clinical Trial Centre: Spanning 350 square metres, the new Centre brings together state-of-the art facilities within an integrated multidisciplinary framework to enable clinical research and implementation of gerodiagnostics and gerotherapeutics.
NUS Medicine Launches New Clinical Trial Centre: Spanning 350 square metres, the new Centre brings together state-of-the art facilities within an integrated multidisciplinary framework to enable clinical research and implementation of gerodiagnostics and gerotherapeutics.