Neurons Hidden to Immune Cells Improve Parkinson’s in Rats
By tweaking genes used by placental and cancerous cells to evade immune detection, scientists have created non-immunogenic neuronal grafts that may help Parkinson’s patients [1].
Sneakiness needed
In recent years, scientists have learned to produce cells via cellular reprogramming, a process in which differentiated cells are driven back to a pluripotent, stem-like state. These are known as induced pluripotent stem cells (iPSCs). The cells can then be re-differentiated into other types of cells and benefit from substantial rejuvenation in the process [2].
This approach has the potential to solve many medical challenges, but the problem of graft rejection remains. When cells come from a genetically different donor (an allogeneic graft), they typically trigger an immune response. Immunosuppressants can reduce this reaction, but they come with significant side effects.
However, evolution has provided some inspiration. In many cases, cells have naturally evolved to become invisible to the immune system, such as placental cells, certain parasites and pathogens, and cancer cells.
The idea of borrowing these cloaking mechanisms to create universally compatible, off-the-shelf donor cells has been around for years [3]. Multiple teams have made progress, and in a new study published in Cell Stem Cell, a group of Australian researchers reports a major advance in rodent models of Parkinson’s disease.
The invisibility cloak
In Parkinson’s disease, dopamine-producing neurons in a brain region called the substantia nigra progressively die off. Dopamine is essential for controlling movement and coordination. As levels fall, the result is the hallmark motor symptoms of Parkinson’s: tremors, stiffness, slowness, and balance issues.
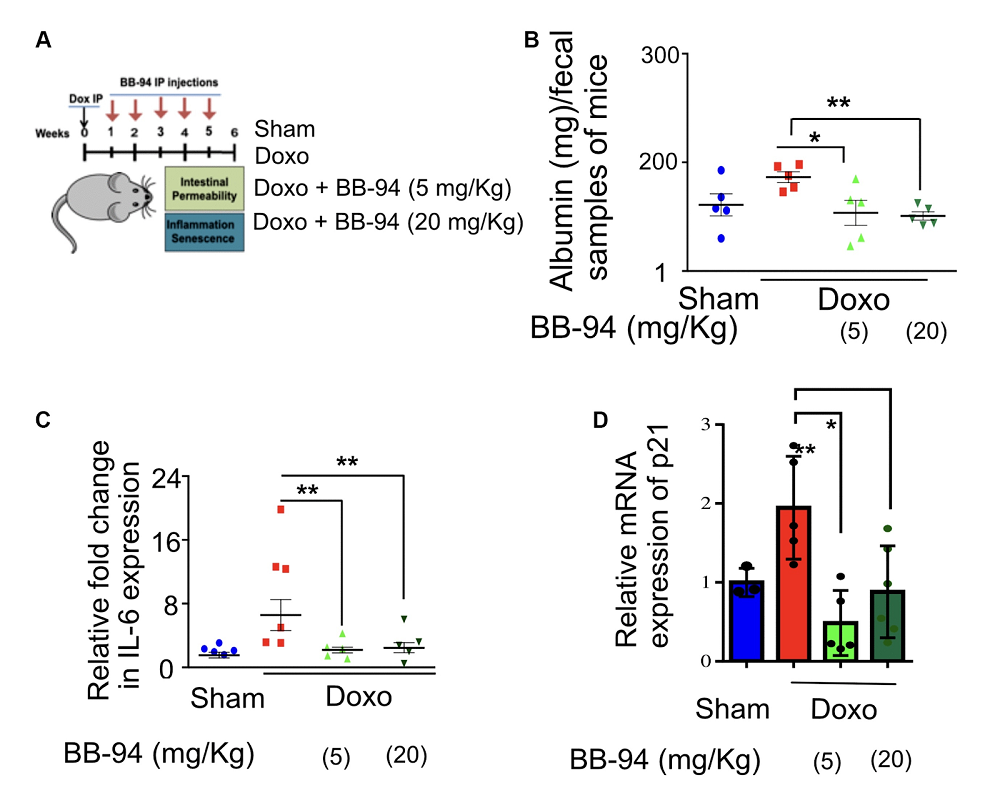
Using cellular reprogramming, the researchers generated neuronal progenitor cells (NPCs) capable of giving rise to new, rejuvenated neurons. These cells were genetically engineered to overexpress eight genes that placental and cancer cells use to evade immune detection. The combination was designed to neutralize nearly all major arms of the immune system: T cells, natural killer cells, macrophages/microglia, and dendritic cells.
However, making cells invisible to the immune system introduces a new risk: if one turns cancerous, the body won’t catch it. To mitigate this, the researchers included a “kill switch” by inserting the gene for herpes simplex virus thymidine kinase (HSV-TK) – an enzyme not naturally found in humans. It was placed under the control of a promoter active only in dividing cells so that any cell that starts to proliferate uncontrollably, which mature neurons typically don’t do, could be selectively eliminated using an antiviral drug.
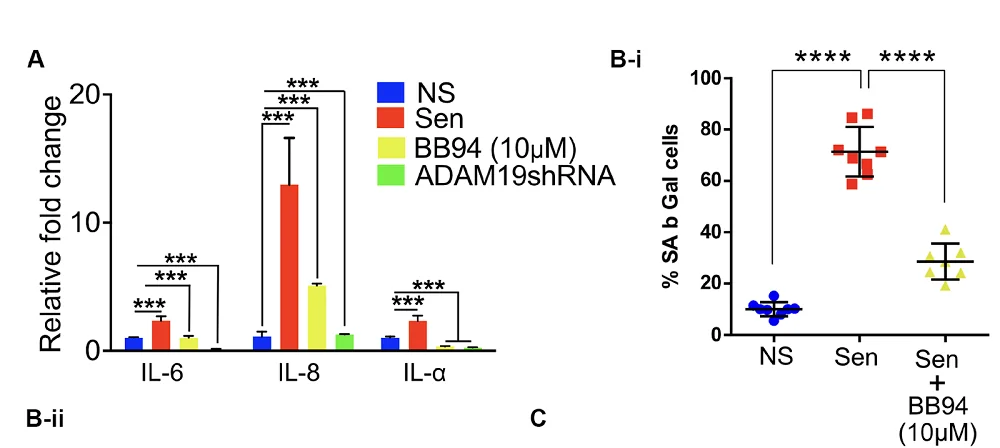
When co-cultured with immune cells from three human blood donors, the cloaked dopaminergic neurons triggered significantly less immune activation, proliferation, and cytokine release. The team then moved to a humanized mouse model with functional human T and B cells.
In this model, uncloaked grafts provoked a strong immune response, while cloaked grafts caused little to no T cell expansion and no rise in pro-inflammatory cytokines. As a result, cloaked grafts grew to about twice the size of uncloaked ones and contained more dopamine-producing neurons.
Functional improvement
To test whether the cloaked neurons could functionally reverse Parkinsonian symptoms, the researchers turned to an immunodeficient rat model of the disease. These rats do not reject either cloaked or uncloaked grafts, so the comparison focused on function, not immune evasion.
Both types of grafts performed comparably: they survived, integrated into the host brain, and reversed motor symptoms by 20 weeks after transplantation. This showed that the cloaking did not compromise the cells’ ability to function.
Finally, the team tested the kill switch in nude mice: animals that lack a functional immune system, making it easier to isolate the effects of the suicide gene. They chose a time point when about half of the NPCs had matured into non-dividing neurons, while the rest were still proliferating. After administering the antiviral drug ganciclovir, the number of proliferating cells dropped significantly while the mature neurons remained unaffected.
“The researchers’ ability to engineer a graftable cell line that can become dopaminergic neurons and evade immune cell targeting fills a gap in the field,” said Dr. Kate Joyce, a researcher at the Lifespan Research Institute. “Not only is the physical process of grafting cells disruptive to the immune system in the brain but in Parkinson’s disease and other neurodegenerative diseases, there is an issue of increased immune surveillance due to a leaky blood brain barrier that further compounds the problem. This method also avoids generating cells from the patients that might harbor harmful mutations and cause more problems later.”
Literature
[1] Pavan, C., Davidson, K. C., Payne, N., Frausin, S., Hunt, C. P., Moriarty, N., Berrocal Rubio, M. Á., Elahi, Z., Quattrocchi, A. T., Abu-Bonsrah, K. D., Wang, L., Clow, W., Yang, H., Pellegrini, M., Wells, C. A., Thompson, L. H., Nagy, A., & Parish, C. L. (2025). A cloaked human stem-cell-derived neural graft capable of functional integration and immune evasion in rodent models. Cell Stem Cell.
[2] Simpson, D. J., Olova, N. N., & Chandra, T. (2021). Cellular reprogramming and epigenetic rejuvenation. Clinical Epigenetics, 13, 1-10.
[3] Lanza, R., Russell, D. W., & Nagy, A. (2019). Engineering universal cells that evade immune detection. Nature Reviews Immunology, 19(12), 723-733.