The authors of a recent paper have reviewed the literature regarding the potential of cannabinoids to treat Alzheimer’s disease [1].
The endocannabinoid system and Alzheimer’s disease
Aging is a well-known risk factor for Alzheimer’s, and more than 50% of people over 85 are expected to suffer from it [2]. There is a need to find an effective Alzheimer’s therapy, since currently used treatments only address its symptoms.
The research found that the endocannabinoid system (ECS) is dysregulated in Alzheimer’s [3]. Review authors speculate that restoring the levels of endocannabinoids and ECS receptor activity can be a potential avenue to prevent Alzheimer’s progression.
ECS has several components, including the cannabinoid 1 receptor (CB1R), the cannabinoid 2 receptor (CB2R), endocannabinoids, and their transport and metabolism proteins. CBRs are naturally activated by endocannabinoids, which include eicosanoids, such as 2-AG and anandamide/AEA.
Aging is associated with changes to ECS. Human and animal studies reported reduced expression of CB1R and ECR-related metabolites in different brain regions [4].
Analyzing postmortem brain tissues from Alzheimer’s patients revealed overexpression of CB2R in glial cells that surround the senile plaques. Additionally, one of the proteins that take part in the AEA metabolism, namely, fatty acid amino hydrolase (FAAH) that converts AEA into inflammatory pathway precursor, arachidonic acid, is increased in reactive astrocytes that surround neuritic plaques. On the other hand, CB1R expression was found to be downregulated in the tissues of the frontal cortex [5].
Since phytocannabinoids, compounds extracted from the plant Cannabis sativa, modulate ECS, the authors suggest that they could potentially be used as therapeutics for Alzheimer’s. Several metabolites of Cannabis sativa interact with the components of ECS signaling. Two major ones are cannabidol (CBD), the major non-psychotropic component, and Δ9-tetrahydrocannabinol (Δ9THC), the major psychotropic component. Both have an affinity for CB1R and CB2R. However, cannabinol (CBN), cannabigerol (CBG), cannabidivarin (CBDV), and cannabichromene (CBC) are also important players.
Cannabinoids as Alzheimer’s therapeutics
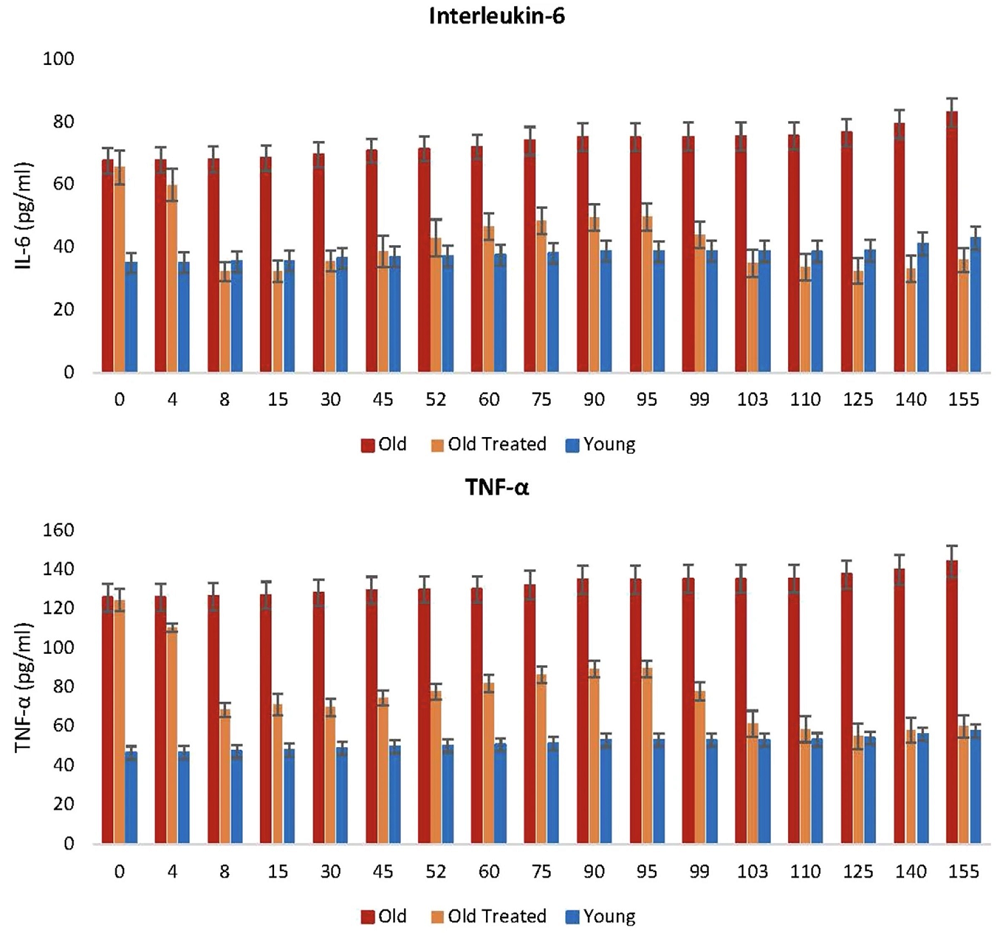
The review’s authors address different aspects of Alzheimer’s and discuss research that has shown that those aspects can be remedied by cannabinoid treatment. First, they address neuroinflammation, as Alzheimer’s patients often chronically experience this. Non-clinical evidence shows that phytocannabinoids can modulate neuroinflammation by their impact on ECS.
Investigation in mouse cell cultures has shown that phytocannabinoids can suppress cytokine production and influence T cell function. In human cell cultures, CBD has shown promise in potentially repairing the blood-brain barrier, which can be disrupted in Alzheimer’s [6, 7].
Similar results were obtained in vivo. Research done in rodents inoculated with amyloid beta has shown that CBD led to a reduction in cytokines and pro-inflammatory mediators. Similar results were obtained with synthetic cannabinoids [8, 9].
The next aspect of Alzheimer’s discussed in the paper is neurotrophic factor signaling. Neurotrophic factors are molecules that regulate synaptic plasticity and neurogenesis and prevent neuroinflammation and neuronal death. Neurotrophic factors include such molecules as TGF-1, BDNF, and Insulin-like growth factor 1 (IGF1).
Research in healthy subjects has shown that acute administration of Δ9THC led to increased BDNF levels. However, chronic exposure to Δ9THC leads to CB1R downregulation and reduces BDNF release [10].
In the early stages of Alzheimer’s, IGF1 levels are increased. Δ9THC and CBD may potentially decrease elevated IGF1 levels; however, this experiment was conducted on a Huntington’s disease model [11].
Effects on plaques
Amyloid beta plaques are one of the main characteristics of Alzheimer’s. Therefore, preventing their accumulation is often a main goal of treatment.
Research in cell cultures has shown that CBD can inhibit amyloid beta-induced tau protein hyperphosphorylation and decrease amyloid beta production [12, 13]. Δ9THC shows similar properties, and it potentially inhibits amyloid beta synthesis and may prevent amyloid beta aggregation [14].
In vitro studies in a human neuron-like cell line suggest that other phytocannabinoids, specifically CBDV, CBG, CBC, CBN, and CBD, can remove already formed and aggregated amyloid beta and stimulate their degradation [15].
When a combination of Δ9THC and CBD was used in mice, there were lower levels of the most toxic soluble amyloid beta form and a reduction of amyloid beta oligomers and tau pathology. Synthetic cannabinoids, when administered in rats, also showed accelerated amyloid beta clearance [16, 17, 18].
Dendritic spine density and morphology was the next main area of focus in this review. Dendritic spines are small protrusions from dendrites. They form contacts with axons of neighboring neurons. During aging, the researchers observed reduced spine volume and length along with lower density of dendritic spines [19, 20].
The authors note the scarcity of research on dendritic spines and cannabinoids. In their review, they noted that evidence from cell cultures and mouse models points to the neuroprotective effects of both synthetic cannabinoids and phytocannabinoids. Cannabinoids have been found to reduce neuronal death and cell gaps and to enable neurogenesis [21, 22, 23].
There were also memory and cognitive tests on mice with amyloid beta-induced deficits. The reviewers noted a reversal in spatial memory and learning deficits along with improvements in social recognition memory and novel object recognition [24, 25, 26].
Pleiotropic effects of cannabinoids and their therapeutic potential
The authors emphasize that there are not many studies on cannabinoids being used as Alzheimer’s treatments. However, the existing data shows the pleiotropic effect of cannabinoids on Alzheimer’s, as it targets many mechanisms and pathways.
Despite the limited research and lack of clinical data, the authors believe that cannabinoids have high therapeutic potential, however, several obstacles will need to be addressed, such as administration routes, as oral administration has variable and low bioavailability.
We would like to ask you a small favor. We are a non-profit foundation, and unlike some other organizations, we have no shareholders and no products to sell you. All our news and educational content is free for everyone to read, but it does mean that we rely on the help of people like you. Every contribution, no matter if it’s big or small, supports independent journalism and sustains our future.
Literature
[1] Fonseca, C., Ettcheto, M., Bicker, J., Fernandes, M. J., Falcão, A., Camins, A., & Fortuna, A. (2023). Under the umbrella of depression and Alzheimer’s disease physiopathology: Can cannabinoids be a dual-pleiotropic therapy?. Ageing research reviews, 90, 101998.
[2] Liu R. M. (2022). Aging, Cellular Senescence, and Alzheimer’s Disease. International journal of molecular sciences, 23(4), 1989.
[3] Tudorancea, I. M., Ciorpac, M., Stanciu, G. D., Caratașu, C., Sacarescu, A., Ignat, B., Burlui, A., Rezuș, E., Creanga, I., Alexa-Stratulat, T., Tudorancea, I., & Tamba, B. I. (2022). The Therapeutic Potential of the Endocannabinoid System in Age-Related Diseases. Biomedicines, 10(10), 2492.
[4] Nidadavolu, P., Bilkei-Gorzo, A., Effah, F., Leidmaa, E., Schürmann, B., Berger, M., Bindila, L., Schmid, M., Lutz, B., Zimmer, A., & Bailey, A. (2022). Dynamic Changes in the Endocannabinoid System during the Aging Process: Focus on the Middle-Age Crisis. International journal of molecular sciences, 23(18), 10254.
[5] Talarico, G., Trebbastoni, A., Bruno, G., & de Lena, C. (2019). Modulation of the Cannabinoid System: A New Perspective for the Treatment of the Alzheimer’s Disease. Current neuropharmacology, 17(2), 176–183.
[6] Kaplan, B. L., Springs, A. E., & Kaminski, N. E. (2008). The profile of immune modulation by cannabidiol (CBD) involves deregulation of nuclear factor of activated T cells (NFAT). Biochemical pharmacology, 76(6), 726–737.
[7] Hind, W. H., England, T. J., & O’Sullivan, S. E. (2016). Cannabidiol protects an in vitro model of the blood-brain barrier from oxygen-glucose deprivation via PPARγ and 5-HT1A receptors. British journal of pharmacology, 173(5), 815–825.
[8] Esposito, G., Scuderi, C., Valenza, M., Togna, G. I., Latina, V., De Filippis, D., Cipriano, M., Carratù, M. R., Iuvone, T., & Steardo, L. (2011). Cannabidiol reduces Aß-induced neuroinflammation and promotes hippocampal neurogenesis through PPARγ involvement. PloS one, 6(12), e28668.
[9] Zhong, C. C., Gao, Y. N., Huang, X. C., Zhu, X., Miao, H. H., Xu, X. G., & Qin, Y. B. (2021). Cannabinoid receptor agonist WIN55212-2 reduces unpredictable mild stress-induced depressive behavior of rats. Annals of translational medicine, 9(14), 1170.
[10] D’Souza, D. C., Pittman, B., Perry, E., & Simen, A. (2009). Preliminary evidence of cannabinoid effects on brain-derived neurotrophic factor (BDNF) levels in humans. Psychopharmacology, 202(4), 569–578.
[11] Valdeolivas, S., Satta, V., Pertwee, R. G., Fernández-Ruiz, J., & Sagredo, O. (2012). Sativex-like combination of phytocannabinoids is neuroprotective in malonate-lesioned rats, an inflammatory model of Huntington’s disease: role of CB1 and CB2 receptors. ACS chemical neuroscience, 3(5), 400–406.
[12] Scuderi, C., Steardo, L., & Esposito, G. (2014). Cannabidiol promotes amyloid precursor protein ubiquitination and reduction of beta amyloid expression in SHSY5YAPP+ cells through PPARγ involvement. Phytotherapy research : PTR, 28(7), 1007–1013.
[13] Esposito, G., De Filippis, D., Carnuccio, R., Izzo, A. A., & Iuvone, T. (2006). The marijuana component cannabidiol inhibits beta-amyloid-induced tau protein hyperphosphorylation through Wnt/beta-catenin pathway rescue in PC12 cells. Journal of molecular medicine (Berlin, Germany), 84(3), 253–258.
[14] Cao, C., Li, Y., Liu, H., Bai, G., Mayl, J., Lin, X., Sutherland, K., Nabar, N., & Cai, J. (2014). The potential therapeutic effects of THC on Alzheimer’s disease. Journal of Alzheimer’s disease: JAD, 42(3), 973–984.
[15] Schubert, D., Kepchia, D., Liang, Z., Dargusch, R., Goldberg, J., & Maher, P. (2019). Efficacy of Cannabinoids in a Pre-Clinical Drug-Screening Platform for Alzheimer’s Disease. Molecular neurobiology, 56(11), 7719–7730.
[16] Aso, E., Sánchez-Pla, A., Vegas-Lozano, E., Maldonado, R., & Ferrer, I. (2015). Cannabis-based medicine reduces multiple pathological processes in AßPP/PS1 mice. Journal of Alzheimer’s disease : JAD, 43(3), 977–991.
[17] Casarejos, M. J., Perucho, J., Gomez, A., Muñoz, M. P., Fernandez-Estevez, M., Sagredo, O., Fernandez Ruiz, J., Guzman, M., de Yebenes, J. G., & Mena, M. A. (2013). Natural cannabinoids improve dopamine neurotransmission and tau and amyloid pathology in a mouse model of tauopathy. Journal of Alzheimer’s disease : JAD, 35(3), 525–539.
[18] Wu, J., Bie, B., Yang, H., Xu, J. J., Brown, D. L., & Naguib, M. (2013). Activation of the CB2 receptor system reverses amyloid-induced memory deficiency. Neurobiology of aging, 34(3), 791–804.
[19] Pchitskaya, E., & Bezprozvanny, I. (2020). Dendritic Spines Shape Analysis-Classification or Clusterization? Perspective. Frontiers in synaptic neuroscience, 12, 31.
[20] Benavides-Piccione, R., Fernaud-Espinosa, I., Robles, V., Yuste, R., & DeFelipe, J. (2013). Age-based comparison of human dendritic spine structure using complete three-dimensional reconstructions. Cerebral cortex (New York, N.Y. : 1991), 23(8), 1798–1810.
[21] Zhong, C. C., Gao, Y. N., Huang, X. C., Zhu, X., Miao, H. H., Xu, X. G., & Qin, Y. B. (2021). Cannabinoid receptor agonist WIN55212-2 reduces unpredictable mild stress-induced depressive behavior of rats. Annals of translational medicine, 9(14), 1170.
[22] Campos, A. C., Fogaça, M. V., Sonego, A. B., & Guimarães, F. S. (2016). Cannabidiol, neuroprotection and neuropsychiatric disorders. Pharmacological research, 112, 119–127.
[23] Esposito, G., Scuderi, C., Valenza, M., Togna, G. I., Latina, V., De Filippis, D., Cipriano, M., Carratù, M. R., Iuvone, T., & Steardo, L. (2011). Cannabidiol reduces Aß-induced neuroinflammation and promotes hippocampal neurogenesis through PPARγ involvement. PloS one, 6(12), e28668.
[24] Cheng, D., Spiro, A. S., Jenner, A. M., Garner, B., & Karl, T. (2014). Long-term cannabidiol treatment prevents the development of social recognition memory deficits in Alzheimer’s disease transgenic mice. Journal of Alzheimer’s disease : JAD, 42(4), 1383–1396.
[25] Coles, M., Watt, G., Kreilaus, F., & Karl, T. (2020). Medium-Dose Chronic Cannabidiol Treatment Reverses Object Recognition Memory Deficits of APPSwe/PS1ΔE9 Transgenic Female Mice. Frontiers in pharmacology, 11, 587604.
[26] Watt, G., Shang, K., Zieba, J., Olaya, J., Li, H., Garner, B., & Karl, T. (2020). Chronic Treatment with 50mg/kg Cannabidiol Improves Cognition and Moderately Reduces Aß40 Levels in 12-Month-Old Male AßPPswe/PS1ΔE9 Transgenic Mice. Journal of Alzheimer’s disease : JAD, 74(3), 937–950.