In this interview with Steve Hill of lifespan.io, Dr. Brad Stanfield discusses the various forms of niacin along with NAD+ boosters such as NR and NMN, and he touches upon supplements, rapamycin, and other facets of the longevity world. Brad is very active in the community and runs the successful Dr. Brad Stanfield Youtube channel.
Steve: Could you tell us a little bit about yourself and what got you interested in aging research?
Brad: I’m a medical doctor from New Zealand, I work in Auckland, and I graduated in 2015. What got me interested in this field was actually looking at the Dr. Sinclair and Joe Rogan podcast. I think that was quite an eye-opener about the things that were coming through the lab and I wanted to create, I wanted to have a really robust resource where people could go to and look at the data and actually make their own decisions.
I realized that a lot of the information that was out there, a lot of it was extrapolated from cell data or mice data. It wasn’t actually looking at the human clinical trials and putting those under the microscope, so I wanted to create a YouTube channel or some sort of portal that people could go to and look at the human clinical trials to see what they could do about their own health and improve their healthspan.
It’s certainly a good thing, because there’s a lot of information out there. A lot of misinformation and old information. That was something that I noticed about your channel; I quite like that you would do a video, and then when there was an update, you’d go back in time and actually mark it outdated, and then you’d point to the newer video.
It made it really easy for me to get up to speed quickly. If only everybody else was as diligent, no names, I’m not gonna name any names, but there’s plenty of channels that are very confusing. What you’re doing is a service to the community.
Now, I’m going to put you on the spot here a little bit.
Do you think it’s plausible that we could bring aging under medical control? If so, what first made you think that this might be possible?
That’s a really good question. I suppose it depends on whether you’re talking about extending lifespan or whether you’re trying to extend healthspan, because there’s definitely a difference. There’s good mice data showing that we can improve, for example, exercise performance, but there’s actually very few therapies that are reproducible in mice that extend their lifespan.
One of the best mice setups is called the interventions testing program, and one of the molecules that they keep coming back to is rapamycin, which extends lifespan by anywhere between 10 and 25%, but there’s very few therapies that can actually extend lifespan in mice in that setup. I’m hopeful that we can find therapies that can extend lifespan, but at this point, I think it’s it’s more valuable to focus on what we can do to improve muscle performance and decrease disease rates in older people, because I think that if we can make sure that an 80-year-old can still do the things that a 50-year-old could do, that’s massive for the world.
It means that the investment that was made, and that person with the education and experience, you could hopefully get another five or ten years of really high-quality work. I think what I’m excited about is actually extending healthspan as opposed to lifespan at this point.
Yes, I think the focus right now is more on healthspan. That seems to be the battle cry of so many people. It’s like the old adage: it’s not the amount of years, but it’s the quality of years. I think that’s a great thing, something to definitely aim for, but I’m greedy, I’m afraid I’d like both. I’d like quality and quantity if that’s possible. I definitely think it’s a good idea to move towards that, initially.
A lot of the therapies that people are working on that are near term, in my view, a lot of those are more to do with healthspan rather than lifespan extension, they’re more likely to improve quality of life and compression of morbidity, they’re more about that sort of thing, so that the period that you spend sick is pushed further to the end. You might not necessarily live any longer, but your healthspan is increased. I think a lot of the things right now that are near completion or even available now in this field are predominantly about healthspan.
I think it’s also easier to measure it in clinical trials as well. If we can find a therapy where, if it’s compared to a placebo, we can say that, in older people, using this therapy, diet, or exercise regime improves muscle performance, and it allows people to walk further and faster, it’s easier to design a trial around that as opposed to lifespan, as well.
I think that it can help older people when medical guidelines can be updated to say older people should be on X, Y, & Z therapy because we’ve got the data to back it up, whereas if you’re trying to design a trial around lifespan in humans, it’s a long time to wait and you’d need quite large numbers to prove that you can actually live longer on a particular therapy. I think, for multiple reasons, it’s probably a good idea that we focus on healthspan.
Some people do say you have to do these longitudinal studies for lifespan in order to see whether something works or you have to wait 60, 70, 80 years before you can know. I think biomarkers and projections are also a reasonable way to proceed.
I think that healthspan is much easier to focus on now, and if we can rejuvenate organs and make them biologically younger, it’s possible that they may live longer anyway, so I wouldn’t worry too much about that at this point. Personally, I think we just need to focus on getting things that work and see where they go. Speaking of which, we’re going to talk about NAD precursors.
Would you say that NAD precursors fall more into the category of things that support healthspan in humans, or would they be something more that might extend lifespan?
I think it’s probably best to discuss the research that’s actually gone on so far in terms of healthspan and lifespan. With NMN, we’ve got a 12-month study that I’m aware of. That was published, I believe, in 2016. In that trial, what’s exciting about it is that the mice were running longer, and they were running faster, but it wasn’t a trial designed to look at lifespan. When you have a look at nicotinamide riboside, which is another NAD precursor, that did extend lifespan, but it was a very, very small extension.
What’s more exciting about that trial, again, is that the mice were running longer, and they were running faster, and they had lower rates of disease. From the mice data, I’m far more excited about the healthspan possibilities as opposed to lifespan, because with the lifespan extension, it was so minute that it didn’t really make much of a difference.
If you look at the human clinical data that we’ve got for NAD, we don’t have data yet on nicotinamide riboside or nicotinamide mononucleotide yet, but we do have a lot of data about niacin or nicotinic acid. This, again, is also a precursor to NAD, but it’s been used in clinical practice for literally decades as a way to improve cholesterol. That’s been largely replaced now because of statins, but we do have a lot of data, looking at niacin.
One of the best pieces of evidence that we’ve got about whether niacin will actually extend lifespan or not is a Cochrane review. Just for people who don’t know about Cochrane, it’s an independent organization that takes all of the clinical trials together, combines them, and sees what the data shows. One of the reasons why Cochrane is held in such high regard is that it’s not for profit and it’s not influenced by big pharma or governments.
There was a study by them published in 2017, and the end conclusion is that we’ve got moderate to high-quality evidence suggesting that niacin does not reduce mortality. That meta-analysis included just under 40,000 people and 23 different studies. I think we’ve got good evidence showing that nicotinic acid or niacin probably won’t extend lifespan, but I’m excited because we do have some clinical data showing that it may actually improve healthspan. That’s where I’m at at the moment.
Speaking of niacin, things do get a little bit confusing with niacin. When you go on Google and look for the supplement itself, there’s a bit of a world of confusion out there already, because you’ve got various things. You’ve got things like sustained-release, slow-release, delayed-release niacins. Not all niacins are equal, because not all niacins are the same thing.
You’ve got nicotinic acid, you’ve got inositol hex as well, which is the no-flush, often marketed as, and niacinamide nicotinamide. I’ve seen all these things marketed as niacin, and my rule of thumb is, unless you go bright red like a tomato and you flush, I know that it’s not proper niacin.
Can you shed any light on the confusion, because so many people ask us which is which?
One of the big side effects of nicotinic acid or niacin is the flushing, as you’ve mentioned. One of the ways that drug companies tried to get around this is by producing a sustained, released version. Essentially, that’s just where you take a capsule that’s time released so it only releases small amounts of nicotinic acid over time. That way, you don’t get that flushing effect. That’s what’s called no-flush niacin. The trouble with that is there is the possibility that you can cause liver damage if you A, take too much, and B, the time release is too long, if the niacin is being released to your body over a really protracted period of time.
The data that I’ve looked at suggests that the instant-release version is probably the safest one. Yes, you get the flush, but it’s probably the safest version. When it comes to the inositol hex, that’s just another way to extend how quickly the niacin is being released to the body. So niacin and nicotinic acid, they’re the same thing.
But then you’ve got nicotinamide, which is also marketed as no-flush niacin, but that’s a completely different molecule that works in a different pathway to boost NAD. As you say, if you’re not going bright red, there’s probably not true niacin or nicotinic acid.
I must be a little bit strange, but I know I’m not alone. I do actually quite like the flush, the flushing sensation that you get. It’s almost like a burn that you get from a product in the UK, I don’t know if you’re familiar with it. It’s called Deep Heat, it’s like a gel, and it basically leaves you with a very similar sensation. I kind of like that, that’s probably weird, I know.
We do get asked quite often what is that flush, because people, sometimes, they’re not ready for it, and it can be quite alarming, especially if it’s your first time taking niacin and you go “Oh yeah, I’ll take 500 milligrams,” and then you’re suddenly bright red.
A lot of people ask us “Is the niacin flush dangerous?”
There’s been a lot of research looking into niacin, nicotinic acid and looking at that flushing effect. This is a molecule that’s been used for decades, and that flushing effect, there’s no evidence that that’s dangerous. It’s caused because of a release of prostaglandins, but that initial burst of prostaglandins is not dangerous and doesn’t seem to be detrimental to human health in any way.
That’s the latest data that we’ve gotten; personally, for me, I can’t tolerate more than 100 milligrams of nicotinic acid. I only take a very small amount because I get very flushed, and I find that it burns if I take more than 100 milligrams. That’s as much as I can take.
I take 500 mg a day. I built that up over a long time, because when I first started, if I took just 50 milligrams, I’d look like a beet root. But now on 500, sometimes if I’ve forgotten to take it for a few days, it kind of almost resets, and then I’ll flush. Sometimes because I like the flush because I’m strange, I’ll actually not use it for a few days, so I can get the flush back. So that’s kind of strange, but I’ve met other people in the community who actually do enjoy it.
It kind of reminds me of almost like the afterglow from during intense exercise as well. There’s a bit of that to it, but I know that it dilates the blood vessels. The vasodilation effect of it, and that actually is beneficial as well. I certainly feel more energized after I’ve taken niacin. I’m climbing the wall like Spider-Man for like an hour. I know something’s got to be working there. I’m 46. So, I’ll take what I can get.
I’ve heard from a few people in my YouTube comment section that really enjoy the niacin flush as well. One of the things that, that I’ve also read in the data is that as you say, a lot of people develop a tolerance to it, so you start with a really small dose and you can work your way up. I’ve tried to do that. I’ve been taking niacin for 18 months now, and I just can’t get past 100 milligrams.
The other downside of using nicotinic acid or niacin, it does increase your blood sugar levels a little bit. That’s another reason not to go completely crazy with the dose. The dose that’s used in humans, I think I’ve read a study that goes all the way up to four grams of it, which is huge. In those trials, they’re using nicotinic acid for cholesterol reasons, whereas here, it’s more for the NAD boosting effect. I can’t see the reason why you’d want to take more than one gram of nicotinic acid.
We know it does modify cholesterols and lipids. We know it definitely works.
Interestingly, on that point, though, coming back to this Cochrane review. Why do we worry about cholesterol? One of the big reasons why we worry about cholesterol is, will controlling cholesterol decrease heart attacks? In the Cochrane Review, there’s no evidence that niacin decreased the rates of heart attacks or strokes, which is odd because it does improve the cholesterol profile.
That brings me to a point that you mentioned about biomarkers. Biomarkers have their place, but at the end of the day, what matters is are people healthier, not does their blood profile look better, but are they actually healthier, do they have lower rates of heart attacks, can they exercise for longer periods, that’s what really matters.
Everybody’s different, because there are genetically different groups of people all over the world, some of them have much higher cholesterol levels than Europeans typically, and yet they’re perfectly healthy. I think you have to take that into account as well. Another potential issue is the methyl group depletion as well.
It’s not necessarily confirmed, but some people do think that it’s an issue that by taking niacin and boosting NAD, it’s depleting methyl groups, which is then starving the body of methyl groups for other things.
Did you want to say anything about the methyl issue?
From the human data, there’s good evidence showing that if you take niacin, it boosts a molecule called homocysteine, which can be indirectly used as the amount of methyl groups that the body has available. Very indirectly, it’s not a particularly good measure, but homocysteine levels do go up. What that may indicate is that taking niacin is drawing from the methyl group or methyl pools that that the body’s got available.
How much of that actually corresponds to human health is very much up to debate, but while we’re in the infancy of all this, starting to find things out, personally, I don’t want to risk drawing away from my methyl pool. There’s different molecules called methyl donors; trimethylglycine (TMG) is one of them. By taking that, you essentially give your body methyl groups, and it just means that you’re not potentially opening yourself up to the negative effects of nicotinic acid.
It’s theoretical; there’s not a huge amount of data behind it. TMG, as I said, is a safe molecule, we know a lot about it, and there doesn’t really seem to be a downside about taking a small dose of TMG while we wait for more data to come through.
I added TMG to my very small list of things I use. I don’t use a lot of stuff; I use niacin, TMG, glucosamine. It’s that 15% reduction of all-cause mortality from those massive studies that’s hard to ignore for glucosamine, but that’s another subject for another time. Homocysteine, ironically, elevated levels are also a potential indication of susceptibility to heart attacks.
Wouldn’t it be ironic that people were taking niacin to avoid heart attacks, but we’re actually elevating their risk of having a heart attack?
That’s a really good point. It seems that if someone’s got a baseline high level of homocysteine, that may be a marker that they are at a higher risk of having a heart attack, but there’s been a lot of research looking into what happens when you lower the levels of homocysteine if you increase folate levels or if you give molecules such as TMG. Interestingly, if you lower homocysteine levels, that doesn’t lower heart attack risk.
It seems that if you do have higher levels of homocysteine, maybe that’s a marker that you potentially need to be exercising more or that your diet needs improving, maybe. Ut looks like if you lower the levels of homocysteine, that doesn’t really correlate to decreased rates of heart attacks, and that’s why in clinical medicine, we don’t routinely measure it, because trying to get targeting therapies to lower it has haven’t really worked out for whatever reason in human clinical trials.
Things like C reactive protein perhaps?
Again, it’s tricky because so CRP is just a general marker of inflammation. When I was working in orthopedics, so bones, one of the things that we use CRP for is a marker of inflammation. If someone comes in with an infected foot, and you want to get a baseline about how potentially bad that infection is, you use CRP.
Measuring CRP in otherwise healthy people, generally CRP goes up as we age, and this is quote-unquote inflammaging, where you’ve got all this inflammation that’s happening in the body, but you’re not fighting an infection at that point. That’s definitely an area that may bear fruit in trying to extend healthspan, but measuring CRP and trying to use that to correlate with heart attacks, again, that’s not something that’s typically done in clinical practice.
So the take-home here is, it’s pretty difficult to work those sorts of things out, but hopefully niacin isn’t actually going to be increasing your risk, and it probably isn’t. Especially if you’re addressing this methyl depletion issue, you mentioned folate is another way, although folate isn’t as efficient is TMG, is it?
You do need enough folate and B12 for for the different cycles, so you’ve got the folate cycle, for example. In terms of actually giving your body methyl groups, TMG is a very efficient way of doing it.
I believe it’s an extract from beetroot; beetroot’s quite rich in TMG. Maybe if you’re eating a predominantly plant-based diet anyway, you probably already get a lot of methyl donors.
Subsequently, you’re probably going to be having low levels of homocysteine anyway if you’re eating a predominantly plant-based diet.
And diet’s a difficult one, there’s no such thing as a perfect diet, but the evidence appears to suggest that a more plant-based, fiber-rich diet does favor longevity. You can’t say there’s a definitive diet per se because everybody’s different, but more the fiber and plant-based food in your diet, I think, is generally a pretty good thing.
People have very strong opinions about diets, and particularly whenever I do a video about diets, it always sparks a lot of controversy. I don’t mean to spark that controversy, I just mean to present the data, but overall, you’re correct that if a higher proportion of your food is plant-based, that probably is better for your overall health, particularly with the fiber component.
Getting back to niacin, what is the evidence? We know it’s a precursor, but what is the evidence that it does actually boost NAD in humans? We know it does in mice.
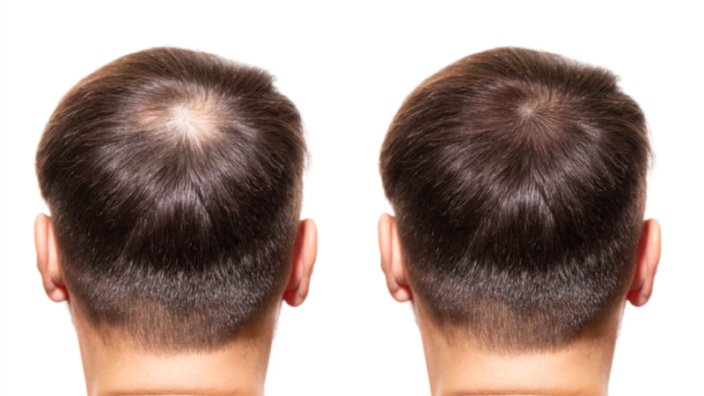
We’ve got very good data showing that niacin does increase NAD in humans. I’m just going to read a trial here, published in June of 2020, and it’s titled Niacin cures systemic NAD+ deficiency and improves muscle performance and adult onset mitochondrial myopathy. What we’ve got is evidence showing that blood NAD increased in all people up to eight times, and muscle NAD also increased with niacin. Importantly, in this trial, muscle strength, and the rate of building new mitochondria, which are the powerhouses of the cells, they increased in the niacin group.
This is a human clinical study, so what I like about this trial is that it’s taking a diseased population, so something’s actually wrong with this population, their mitochondria aren’t functioning in the optimal way. The study was looking at using niacin and compared it to placebo to see what would that do to muscle performance and mitochondrial performance, and we’ve got good data showing that niacin improves mitochondrial performance in that disease population.
For me, that’s really encouraging because as we age, our mitochondria, they’re not as efficient as what they once used to be. If we can use molecules that boost NAD, such as niacin, to improve mitochondrial performance, maybe that will improve muscle performance and thereby extend healthspan. The human clinical data coming through about boosting NAD, I’m very excited for, and there’s a lot of clinical trials happening right now that I can’t wait to read when they eventually come out.
It’s interesting, I’d like to see similar studies with other types of tissues to confirm whether it does enter those cells as well. It could be very cell specific, but it probably isn’t. We can’t say that until we’ve got the data. I’d love to see the tissue, brain tissues as well. I’d love to see heart tissue and heart cells and and see how it compares.
It could also be very low-hanging fruit for combating frailty, sarcopenia, things like that, that rob people of quality of life and their independence as they get older. It’s cheap, because it’s obviously been around, it’s been very well studied. I don’t even know when the patent ran out on it, but I’m guessing probably 50 years ago, 60 years ago maybe, because it’s been around for a long time. It’s a no-brainer if it works, and it’s safe, relatively speaking.
You’re right, it has been around for ages and it’s vitamin B3. It was initially used to treat pellagra, low levels of vitamin B3 cause it. It’s a triad of dermatitis, dementia, and death. Foods were fortified with vitamin B3 or niacin to combat that.
If it increases NAD, why would we take NR or NMN? Why bother? I mean, it’s expensive.
Both of those molecules are more expensive, but they probably have a couple of advantages over nicotinic acid. The first and foremost being, they don’t cause flushing and they don’t cause increases in homocysteine levels, so there’s mice data showing that there doesn’t seem to be an issue for whatever reason, so maybe just because of the mechanism of action, they draw on the methyl pool less compared to niacin, and they don’t cause increases in blood sugar levels.
There’s also some mice data showing that if you give equivalent doses of niacin, or NR or NMN, NR and NMN seem to boost NAD more compared to nicotinic acid, so there’s potentially a couple of advantages. I’m not aware of any human clinical studies that directly compare these molecules in terms of muscle performance and fatty liver.
I think that’s what’s really important is that we focus not necessarily so much on the biomarkers but what does it actually do to human health. What’s it doing to your exercise performance, fatty liver. Those potentially would be the reasons as to why you might go for NR or NMN, that there’s potential benefits.
We need a comparison, a big study where we put them all head to head, we can use biomarkers. Ideally, functional aging biomarkers would also be a thing that I would use, so their ability in real life terms. Get up from a chair, this is a biomarker that some people use; getting up off the floor, how quickly you can do that has been linked to mortality. Obviously, they could use functional things like that, just getting to the shops, the six-meter walk tests and things like that, those could also be incorporated into a trial along with chemical biomarkers, blood works.
I think it’s important to combine those two, because as you say, quality of life is the aim here, not just blood works, not just biomarkers in the blood. That could work, but is anybody doing it? Maybe that’s something that we should think about trying to organize at Lifespan.
I suppose; it’s that the devil’s in the detail with designing a trial like that. As you’ve mentioned, you have to design it correctly and just for people who aren’t aware of how clinical trials are run, a well-run clinical trial would have some form of placebo as one arm of your trial, and you want overall to have a primary outcome. If you had to choose only one thing that you want to see if there’s an effect, what would you choose, and then you power your study to that, making sure that you’ve got enough participants in your trial to actually see whether there’s an effect and you get a statistically significant outcome.
My concern is that to power a study that directly compares NR to NMN, if you’re looking at muscle performance, you would have to have hundreds if not thousands of people to see a true difference, and that would be incredibly expensive to do in humans. What I think is more important is, first of all, we test whether one of these precursors to NAD does improve muscle performance or does improve hearing loss, or it makes your hair or nails grow faster compared to placebo, those are things that I think are really interesting. But to power a study that directly compares NR to NMN with a primary outcome of muscle performance, it would be incredibly expensive to do.
I do feel that there definitely, at some point, must be a reckoning. We’re certainly always asked which is better out of these three, and the truth is we can’t say because the correct studies just have not been made yet, so I think it’s got to happen. I know it’s going to be expensive.
We’ve only got so many resources when it comes to clinical trials, and the expense involved in running a clinical trial that’s well designed and well conducted, is that the best use of that limited resource to directly compare NR to NMN or nicotinic acid? If we can find out one of those molecules, improves muscle performance, does it matter to get to compare all of them to see which one gives a very slightly increased benefit, or is it better to use that resource to study other molecules?
That is true. They all boost NAD. We know that, you know there’s going to be some benefit. Then it may be possible to work out what’s most efficient, but let’s just put it this way, Grandma takes them and suddenly benches 180 kilos, does 50 reps, I’m going to be a bit suspicious that something’s working there, but you’re probably right, we’ve got to be smart with the limited resources we’ve got, and it’s probably going down the rabbit hole trying to get dig too much into the details.
Speaking of human trials, NMN, what’s the level of evidence for that in humans? We know all about mice, it’s quite beneficial in mice, but what about humans?
There’s been a couple of trials that have come out showing that NMN does improve NAD blood levels. One of the trials looked at insulin sensitivity and claimed that NMN improves insulin sensitivity. There is a problem with that study. Ideally, when you do a trial, you want both populations or both groups to be roughly the same, and that way you can see will your therapy actually work, so you’re comparing apples to apples.
One of the groups in that trial that looked at insulin sensitivity and NMN had significantly worse liver health. One of them had significantly higher rates of fatty liver, and that’s a problem because one of the theories is that if you take NMN, one of the first tissues that will have an effect, or you’ll see a benefit, is the liver. If one group has got significantly worse liver function, it’s very difficult then to start looking into insulin sensitivity. I think the jury’s still out on whether it does improve insulin sensitivity, but we do have human data showing that NMN does improve NAD blood levels.
Of the precursors, it’s probably the one that’s lagging behind the most in terms of actual human data. NR is, it was a good year or two before it appeared, so it’s got a lot more behind it, but I think NMN is interesting. Some people have suggested, and I don’t know whether you want to venture an opinion on this, that the NMN molecule itself is too large to enter the cell, and there’s talk about, it has to convert back into NR before it can enter the cell. I wondered if you had any thoughts on that at all?
I suppose all I can do is just mention the controversy around this. In 2019, there was a study published saying that there’s a particular transporter of NMN. Overall, just for people who are new to NAD, what we’re trying to do is boost the NAD levels in the cell. You need to figure out a way to actually get your NMN or whatever molecule you’re trying to convert into NAD into the cell in the first place.
There’s a well-established pathway where NMN gets converted to NR, that NR then gets into the cell and then gets converted back into NMN, that’s been known for quite some time. This 2019 paper kind of shook things up because it was suggesting that in mice, we could directly get the NMN into the cell.
Now, I’m not a biochemist. When that trial came out, there were one or two papers, or comments that were published, suggesting that this trial had some methodological issues and that the data that they were presenting was less than ideal.
Again, I’m not a biochemist, so I can’t really speak towards that. I don’t know if NMN is directly absorbed, I think again, coming back to it, what’s most important is what does NMN actually do to human health? Will it improve fatty liver, will it improve muscle performance? I think that’s more interesting as opposed to this presumed transporter.
Even that aside, even if it does have to convert back to NR, we know that it reliably boosts NAD levels. We’ve seen in animal studies that it does it rapidly. You give a mouse NMN, then its markers for NAD production increase, and it happens so fast that it seems that even if that was an additional step, and it had to go back to NR before it could get in, it doesn’t seem to really hamstring it in any way, it doesn’t seem to stop it working. You’re probably right. Does it really matter? Maybe not.
I suppose this is tricky, because there’s an interesting fact that I don’t think many people appreciate, it’s that 95% of promising therapies in mice don’t translate to humans. So, when they’re tested in humans, there’s either no effect, or significant adverse effects, and the trials are stopped.
When it comes to these NAD precursors, one of the hopes is that it improves muscle performance and that it improves muscle NAD levels. We’ve got a trial looking at nicotinamide riboside that, whether the trial didn’t go on for long enough, or maybe it needed to be paired with exercise as well, I don’t know, but the muscle NAD didn’t go up. There were other metabolites that did, but actual NAD didn’t go up.
It’s tricky to know what to make of that data, and that’s why I think it’s just really important to pair these molecules with a great diet and regular exercise, and particularly with the trials, powering the trial to look at muscle performance, will this actually make older people walk further, and will it make them have a stronger grip strength? I think those are the really key markers that we need to measure.
What we would call functional aging biomarkers. A few years ago on Lifespan, we funded a device a few years ago called the AgeMeter. It’s used to test things like exhalation, your ability to grip, and hearing, all these sorts of very basic functional tests. They’re very, very good indications of how healthy you are in general.
As I mentioned earlier, the test of literally rising out of the chair, it’s very valid because some people are faster than others. Those sorts of things also relate to daily life; so what if someone’s got more C reactive protein in their blood? We’re more interested in whether Bob can get to the shops easier than he could six months before. I think you’re definitely right, functional biomarkers should be used a lot more in the context of what we’re doing. The jury’s really out on that.
Just one thing about the point that you’ve raised about functional biomarkers: One of the things that is really hot within this healthspan and lifespan field at the moment is DNA methylation clocks. I think they’re an interesting marker.
However, I don’t think that they should be used as reasons for why a particular therapy is good or not. For example, if you use these DNA methylation clocks, and you give one group NR, and the other group placebo or NMN, and you find that the NR or NMN group have lower levels or have improved DNA methylation parks and use that as evidence for their use, I don’t think that that’s right.
It’s not going to translate into clinical practice, because the clinical guidelines that they want to know, in terms of function, what will this therapy do for older people, and will it improve their muscle strength and performance? That’s what’s really exciting about these therapies, is that, will it improve muscle performance? Using DNA methylation clocks, again, it’s interesting, but I don’t think they should be the primary outcome of any study.
They’re definitely a useful biomarker. Some people would say that they were the gold standard for aging, I would say that we don’t really fully understand methylation clocks, because there are so many different ones. There’s the Horvath clock, there’s the GrimAge, there’s the PhenoAge, there’s loads of them, but it’s not always entirely clear what they’re actually measuring. We know that it’s related to aging, but what is it related to specifically?
I don’t think it’s well understood enough at the moment to really be used as the only sort of way of measuring the outcome of anything. Certainly, you could use it in unison with a panel of other biomarkers, but I agree with you there, I don’t think it should be used as a sole thing, because I’ve seen a few studies, and they just use that and it’s like, “Hey, it works.” and I’m like, “What worked? Did it improve someone’s quality of life?” Valid point about that, I think that’s one of the big issues that the field faces is actual biomarkers that will be accepted to get therapies into human trials and approved, and I think that’s a big problem.
Functional aging biomarkers, I think should always be included in human trials, as you say quality of life, and another vaguely controversial topic: You don’t have to say anything. It’s fine if you’d like to say no comment.
I’m going to ask you about sublingual NMN. This seems to be very trendy in the supplement community here, a hipster way of taking it, but what does the data really say about sublingual delivery?
This kind of kicked off after a 2018 study published by Liu et al, and it’s titled “Quantitative Analysis of NAD Synthesis-Breakdown Fluxes“. Essentially, what this trial wanted to figure out is, how is NR, NMN actually absorbed into the body, and how is NAD built when these molecules are supplemented? This was a mice trial, and what they did is isotopically label the NR and NMN.
Essentially, that just means that you’re putting markers on the NR and NMN that you’re supplementing to see what actually happens to these molecules. That allowed them to figure out is the NAD being directly made from the supplements, or are the other pathways happening? What they found is that both of the NR and NMN were quickly degraded into nicotinamide in the whole blood, and this was irrespective of whether you gave it IV or whether you gave it orally.
What seemed to be happening is that the liver was breaking down NR and NMN into nicotinamide, then it was the nicotinamide that was boosting the NAD in these mice. Nicotinamide’s a very cheap molecule, it does boost NAD, but it possibly doesn’t do it as well in theory. It wouldn’t do it as well as if the NR, NMN were directly absorbed, and there’s also a potential impact.
It’s that if you’ve got too much nicotinamide, that may inhibit some enzymes such as sirtuins and PARPs, which are involved in DNA repair and health, so on the back of that, the theory was that maybe if you took NMN under your tongue, you could bypass the liver, and you could directly get the NMN into the blood and then distributed around your body.
When I used to take NMN, that’s what I did, I put it underneath my tongue, but there’s definitely no human evidence that that’s a better way or gives better outcomes compared to just swallowing normally, and given that NMN does get degraded in the blood quite quickly, even if you could quickly get it into the blood, would it actually improve your muscle performance compared to if you just took it normally? It’s probably unlikely, to be honest.
That’s where all of this came out now. When I spoke to Dr. Charles Brenner about this, who knows a lot about nicotinamide riboside in the NAD metabolome, he thought that we shouldn’t put too much weight into this data because from his lab, that’s not what they came up with.
Again, I’m not a biochemist, so I can’t really comment to that. If you did want to take it under your tongue, there’s probably no harm in it. Is it going to give you much benefit? Who knows. We don’t have that data yet.
I’m a bit old school, so I just take a pill. We just don’t know, but it seems to have been become very popular within the last year or two, and everybody’s now got one of these sublingual products, but as you say, we need more data on that. I even see that there are some places that are doing NAD therapies, they put it straight into you via an IV.
But NAD is a very large molecule, right?
That’s the thing, and it comes back to what we mentioned earlier. Ideally, we want to boost NAD in the cell. It’s not necessarily the blood vessels that we want, or the blood that we want the energy to be high in, it’s the cells in our muscles. Injecting NAD, that needs to be broken down, to be absorbed by the cell.
It’s likely broken down into nicotinamide, so it seems like a very expensive way of just taking nicotinamide. I don’t think it’s got much benefit. I think a lot of people are spending a lot of money, and it’s being marketed very heavily. I wouldn’t go down that path if it’s me.
We’ve talked about NMN and niacin quite a bit today, but we haven’t really talked about the elephant in the room, which is NR.
What’s the evidence level for NR in humans?
We’ve got really good human clinical data showing that it improves blood NAD. We’ve also got a suggestion from a paper that I mentioned earlier that NR likely improves the muscle NAD metabolome. NAD in the muscle didn’t increase in that paper, but all of the other metabolites of NAD did increase, so it’s likely that NR would improve the NAD metabolism in muscle, and that’s essentially it.
We’ve got a lot of safety data, which is great, but we don’t have data showing that it definitively improves fatty liver or that it definitively improves muscle performance, those trials are happening at this stage. What we do have is, if you combine nicotinamide riboside with a couple of other molecules, there’s been a couple of papers that look at this concept called combined metabolic activators.
In COVID-19, for example, your metabolism comes under attack. The theory is that if you can make your NAD or your metabolism more resilient, then you can weather that attack a little bit better, and you should see that in terms of recovery time from infections such as COVID-19.
There was a study that was published showing that in people that needed hospital treatment from COVID-19, if you gave them nicotinamide riboside as well as a couple of other molecules, and you compared that to placebo, the NR group, they recovered three days faster. They could be discharged three days faster, which is huge, and it leads us to think that with this therapy and with boosting NAD, it likely does help human health, particularly when our metabolism is under attack. So that’s a pretty interesting trial.
It is. You say there’s some more studies in flight at the moment, which should give us data for NR. NR is obviously the most in the spotlight because it came before NMN. I know from the reporting that we’ve done that there are other potential approaches to boosting NAD.
There’s the de novo pathway; some people think that that could be enhanced. Any thoughts on that?
Essentially, that’s where you take tryptophan from the diet, and that, through multiple pathways, gets converted into NAD, but that pathway generally links up with the pathway for nicotinic acid or niacin, the Preiss-Handler pathway. I’ve never really got that excited about it, to be honest, with tryptophan. I think there are other molecules that we can use.
That’s kind of my thoughts on it, but again, we don’t have direct human clinical data comparing these molecules with muscle performance and fatty liver and other times that our metabolism is under attack, so we don’t 100% yet know, but my best guess would be that there’s other molecules that would be more efficient at boosting NAD than tryptophan.
Yeah, it doesn’t seem the most efficient pathway but it’s interesting that some people have experimented with it. So, and the other one, which you don’t hear a lot about at the moment because it’s very, very new, is reduced nicotinamide mononucleotide, or the really catchy name of NMNH. Did you see the study, last year with NMNH?
I did. There was also a study looking at NRH. Essentially, it looks like those molecules increase NAD very, very efficiently and very well. But even in the NMNH study. If you have a read-through, it says that NMNH is converted into NRH, and then it gets into the cell. The NRH study also said the same thing.
The trouble with NRH is that it’s very unstable. Trying to supplement it is nigh on impossible, because by the time you try and supplement it, it would have broken down into something else. It’s interesting, but be aware that the NMNH has converted into NRH, and then gets into the cell, but it doesn’t really matter because it’s unstable. So, whether it’s actually going to have any clinical use is unlikely.
That’s fair, I thought I’d mention it because it’s not something that people often talk about, but there are other things in the works. Other ways of boosting NAD levels have been suggested: reducing the activity of our old friend CD38.
You’ve got things like apigenin, which I quite like because I like camomile tea. There are a few other candidates out there, the idea being if we reduce this CD38, then the burden on the pool of NAD that we already have is reduced.
What are your thoughts on actually getting rid of the CD38 as a potential approach instead?
Yeah, so there’s mice data showing that when CD38 is knocked out, as in the mice cannot produce CD38, NAD levels go up. The trouble is, when you do that, the mice encounter all sorts of issues as well. It looks like you don’t want to completely knock out CD38. I’m not sure if it’s mice or human data that shows this, but CD38 increases, I’m pretty sure my study shows that, I don’t know if human data shows it.
CD38 seems to chew up or use up NAD, so the hope is that if you can make sure that your CD38 levels don’t go up, then your NAD is less taxed, therefore you can use it for other other things. It’s interesting, and I’m excited to look at molecules such as apigenin and that will lower CD38.
But, again, what is that actually going to do to muscle performance and fatty liver, and all these other things? I’m hopeful for it. We just need more data, and I keep referring to that during this podcast, but we do need a lot more studies into this, and studies are happening, but they just need to accelerate.
They are, and I remember the Sinclair study where they actually looked at apigenin and quercetin as well. Quercetin, of course, is another naturally occurring molecule, and of course it was part of Kirkland’s senolytics studies. I have a hypothesis that senolytics may be useful in the context of raising NAD because CD38 is a constituent of SASP.
I think if you can actually reduce senescent cells or inhibit SASP, in other ways remove it, I think you’ll see some bounce-back with NAD, just getting rid of that inflammation storm that the senescent cells are causing. That’s what struck me from the 2012 paper with apigenin, quercetin, and other things, was it plutonium? It was something like another polyphenol that reduced CD38. My thoughts are that in reducing SASP and senescent cell burden, we may also see some bounce-back of NAD naturally.
Yes, senescent cells is a really interesting field, but there’s significant challenges with it. For example, senescent cells, they do have a role to play in health. For example, in wound healing, the concept of senescence is vital for appropriate wound healing and some forms of senescent cells do appear to be good, you don’t want to remove them, whereas other senescent cells likely worsen the situation in terms of human health.
It’s really tricky to know which senescent cells we should be removing and which we should be keeping. That’s issue number one, and then issue number two is, even if you can identify that you want to remove certain senescent cells, how do you do that, it’s incredibly difficult. It’s like trying to remove cancer cells, and trying to remove cancer cells is very, very difficult. I’d mentioned that we’re probably going to have the same challenges with trying to remove specific senescent cells. I’m excited about the idea, but there’s a heck of a lot of work that still needs to go on.
There is, and I’m gonna be a bit contentious here and say that I’m actually not a huge fan of senolytics. I think there are other solutions. The best solution, and I’ve spoken to other researchers about it, they seem to think that if we can actually rejuvenate the immune system itself, the immune system knows how to deal with them anyway.
That seems to be the most elegant way of dealing with it, is get the immune system to do it, rather than actually just dumb firing, destroying everything and then, as you say, risking causing all sorts of problems. We spoke to Judy Campisi a few years ago, and she was saying that senescent cells, there’s so many different types, and they all do different things, they’re in different ratios in different tissues, and they’re all using different pro-survival pathways like BCL-w, p56, and some of the ones that I can’t think of right now, but they’re all using these different ones. No one senolytic is going to get rid of them all, and probably you shouldn’t do that anyway. I think there are probably better solutions.
Another one that I saw that recently, which really is exciting, is by Professor Lorna Harries at Exeter University. She and her team are actually experimenting with splicing. What they found is that they restore splicing in senescent cells, aged cells, they start to work like normal cells again, and they’re healthy again. That’s also another potential way of dealing with senescent cells.
That’s interesting because senescence does play a play a role in stopping cancer growth. I’ve always been kind of skeptical about therapies that restart senescent cells. Generally, senescent cells that have previously gone through a lot of cellular divisions and may have picked up DNA mutations and whatnot, and senescence acts to stop that cell from continuing to divide and thereby, in theory, stop cancer progression. I’ve always been kind of skeptical about if you just rejuvenate senescent cells.
That’s always the concern, it’s the concern around telomerase activators as well. If you go back even further to the work of Maria Blasco and so on, often people said it’s not a good idea to bring senescent cells back into the cycle. Presumably, they’re going to have to build some kind of fail-safe system into it, but there’s got to be a way of dealing with senescent cells.
Honestly, I think the money is on actually using your own immune system to do it, because that’s what it’s designed to do. There’s some promising research in rejuvenation of the immune system as well, which is pretty exciting. The thymus rejuvenation by Greg Fahy is one example, you’ve got the mTOR approach as well by Samumed, they’ve changed their name now, there’s quite a few, resTORbio was another one, they’ve changed their name.
There’s some interesting stuff happening on the immune system rejuvenation front. I’m all for having as many arrows in the quiver as possible because senolytics, it could work. It could be made to work. Senomorphics, ditto. I think at this point, the more shots on goal we’ve got, the more chance that something will go in and will score. I think it’s too early to laser focus on one approach.
You’ve touched on something, that this is extremely complex, and trying to simplify it by a blanket rule of all senescent cells are bad is just a complete oversimplification and is going to do a lot more harm than good. Solving aging is tricky, and that’s why one of the things that I try to impart to anyone who’s watching or reading about this podcast, just be extremely skeptical about any claims that you see on social media.
We are, I think, a long way away from solving aging, there’s promising therapies about extending healthspan and improving muscle performance in older adults. I’m very excited about that, but in terms of people claiming that we can live to 200 years old. We are a long way away from that at this point.
I would tend to agree with you there; I think it’s going to happen in stages anyway. I think the first approach is probably going to be tweaking metabolism, making people age better, so your low-hanging fruits. I’m very excited about things like partial cellular reprogramming, because I think they have absolutely massive potential, but I’m also under no illusions that I think this is going to happen next week, because it’s just not.
We’re a good, probably 10 probably 20 years away from seeing such radical or potentially transformative approaches getting into human trials, I think the stuff that’s more likely now is the stuff like NMN, the precursors, and things that seek to rectify metabolism. I don’t think we’re gonna see anyone being 200 just yet.
I know from covering the field how slow science is just because by its very nature, it has to be in some respects. I don’t like to be the bearer of bad news, but we’re not going to defeat aging a week next Friday, it’s just not gonna happen. But we’ll get there, I think, eventually.
I suppose that’s the thing, there’s no guarantee that we will. Every day, we’ve got many trials coming out, and in the medical world, one of the big game changers is SGLT2 inhibitors, which was primarily designed as a diabetic medication, and essentially how it works is that it makes you pee out sugar, and there were some awesome results in terms of protecting the kidneys and the heart against the effects of diabetes.
I’m prescribing these in my clinical practice, and we’re getting awesome results. Now it’s actually being used for if people aren’t diabetic, but they’ve got heart failure, for example, and introducing these medications for heart failure is looking fantastic. There’s many therapies that are exciting and that are coming through that look like we will be extending healthspan. Whether we solve lifespan, I don’t know.
I think that’s fair to say. I think to say otherwise it wouldn’t be right; it’d be unfair, it’d be misleading to say that, oh, we could definitely do it. But, it’s like we say, we’ve got to try, because if we don’t try, we know what the alternative is. Let’s do what we can, but I definitely think that you’re gonna see a lot of these things that are addressed.
Metabolism first, and that may just lead to more healthy years, which is a good thing. Perhaps it might allow you to live five, ten years longer, which is okay because that’s five, ten years longer that medicine has to advance. People always say “Oh, what can I do now?”
There’s not really that much you can do now to increase your odds of longevity. It’s pretty much what your granny would have taught you: get good-quality sleep, eat a sensible diet, do some exercise. Those are pretty much all the things, maybe make some informed choices about supplements.
Obviously, you’ve put the time in and you’ve done the research, I wish more people would do that, because it frightens me when we write about stuff and someone says, “Where can I buy it?” This is in mice, you shouldn’t do that!
You do take NAD precursors yourself, you’ve tried a few, but what are you taking now, what works for you?
As I mentioned before, I’m taking niacin, 100 milligrams, and I take TMG alongside that. When I reach my mid-30s, I do plan on adding in nicotinamide riboside unless there’s new data that’s come through suggesting that another molecule is is better. I take omega-3, and that was primarily because of a meta-analysis that came out last year from the Mayo Clinic, and what’s different about that meta-analysis is that it only included studies where omega-3 was actually supplemented.
A lot of the other meta-analyses included studies that looked at dietary advice, so increasing oily fish. In this meta-analysis, there was a benefit in terms of cardiovascular risk. I take omega-3, also take vitamin D, I think it’s about 3000 or 4000 units a day. I take vitamin K too, but a very small dose of that.
Creatine, I don’t understand why people wouldn’t take creatine, to be honest, that’s the molecule that there’s good evidence showing that it improves muscle A, performance and B, recovery, and there’s also some evidence suggesting that it improves brain function as well, so it’s a molecule that’s been well studied, we’ve had it in supplements for a really long period of time.
I take creatine, and I take melatonin, very small dose. Things like hyaluronic acid and collagen, I take as well. There’s a bit of a list, and I’ve got that published in all of my YouTube videos, so you can have a look there. Those are the molecules that I take.
So, no love for glucosamine? That actually surprises me because the those two really large scale, human-studies, and they got a minimum of 15% reduction of all-cause mortality from the data, and it’s cheap.
When I went through that data, I can’t remember it off the top of my head, but I remember thinking that there were a lot of confounding factors that may have skewed that data. Overall, I thought it was interesting, but I didn’t think that it was by any stretch guaranteed that we were going to be seeing those results. One of the big confounding things, for example, people taking glucosamine over a long period of time generally would A, be wealthy and B, probably know a bit more about health, compared to someone who isn’t taking supplements, just as a general assumption.
That’s a confounding factor, because you’ve potentially got one group that’s going to be healthier anyway, compared to another group. I remember going through the paper, and there was a list of three or four things that I thought could have skewed the data. I think it’s interesting, but I don’t think it’s guaranteed at this stage, and you’re right, it is a cheap molecule, but for me, there wasn’t enough there to start taking it.
It is really dirty cheap over here, so I make a part of what I take, but I don’t take very much.
It’s probably not going to do any harm. Let’s put it that way.
Definitely agreed on the creatine. I used to take that quite a lot when I used to do a lot of running, and I remember seeing there were a number of studies in marathon runners, and it definitely sped up the recovery rate after a marathon. It does seem to support wound healing, and you can absolutely work harder and stronger with creatine. The data on that is irrefutable.
It’s been around for about what 60, 70, 80 years, a really long time; in fact, I think I remember seeing some accounts from the turn of the century, circa World War One, where people were taking it and talking about working out, and they commented at the time that they were able to lift more weight or do more reps. Again, it’s pretty cheap, and the bodybuilding community has known about it for years.
There’s so much stuff out there that you could have a stack a mile long. The problem then becomes all the potential interactions, and that’s what puts me off, because I’ve seen people with stacks, they’ve got a list of supplements a mile long, it’s on a spreadsheet, and I’m like, “But how is it interacting with each other and are you measuring your bios?” and when I ask they say “Oh no, not really, I’m just taking it.”
To me, when people are not quantifying and measuring, and they’re taking that many supplements, it’s kind of almost like faith healing, because they’re just throwing everything at the wall and seeing what sticks, if you’ll pardon the phrase. It’s crazy.
To your point that you said earlier, the stuff that we know makes a difference is diet, exercise, and sleep. I think if people can take anything away from this talk, diet, exercise, and sleep is where the money’s at right now, everything else, yes, there’s trials going on and it’s exciting to talk about, but you can’t get away from diet, exercise and sleep.
There’s some good data for things like fasting of various types, caloric restriction, but I wouldn’t do that, it’s like the ninth circle of hell. This compelling data, not for life extension in humans but in model animals, and, in humans, benefits seem to be improvements to stem cells and all sorts of things. If you can do it, or fasting, it’s worth considering.
Another thing that I recently found out and did a lot of research on and found fascinating was saunas, the activation of heat shock proteins, FOXO, and various other things that are triggered by that exposure to the heat. We don’t have a sauna here. Believe it or not, I bought a spa, which reaches 40 degrees [Celsius] and I’ve seen some papers and I’m glad to say that 40 degrees is just about enough to activate those heat shock proteins, it’s not as good as a sauna. But I figure, well, it’s worth including or considering, if you’ve got the means to go to the sauna.
There was a lot of large studies in Finland a few years ago where they showed there was a big reduction in cardiovascular and all-cause mortality. Through regular use of saunas, so that if someone was using it every day, they were much less at risk of dying, regardless of age, than someone who didn’t or maybe used it once a week. I think that’s something that you could consider looking into.
Some people like cold therapy; I don’t fancy that. I think it’s those heat shock proteins, that hormetic response, which is supposed to have some benefit, but I’m not getting cold for science. No thanks, it’s cold enough.
There’s all sorts we can do, but more research needed as always, keep an eye on what’s going on. Hopefully, the rapamycin pans out. I’m pretty optimistic about rapamycin being effective or other, related rapalogs. I think the data so far is interesting. That was the PEARL trial launched earlier this year, and that was thanks to the community putting a lot of money behind the fundraiser we did on lifespan.io.
I believe you’ve also got some thoughts and where we should go with rapamycin as well.
I’m very excited about rapamycin, and I commend the team at PEARL and lifespan.io for actually getting that trial underway. I think that’s awesome that there’s a platform now where the community can actually contribute to these clinical trials. I think that’s awesome.
There’s a couple of things that I really want to test with rapamycin that the PEARL trial, just because of how it’s designed, won’t answer, and I’m hoping that the trial that I’ve got in mind will because I’m at the infancy of developing that study design. At this stage, I can’t talk too much about it. I’m very excited about rapamycin and rapalogs, but I will have to head off, unfortunately, I’ve got a clinic I need to get to, but this was a pretty awesome talk, so thanks very much.
It’s been really great, we’ve touched on all sorts of things, and hopefully when you’ve got the study design formalized, you’ll have a chat with us and we’ll see what can be done. Thanks for your time and your thoughts, and we’ll hopefully do this again soon.
We would like to ask you a small favor. We are a non-profit foundation, and unlike some other organizations, we have no shareholders and no products to sell you. All our news and educational content is free for everyone to read, but it does mean that we rely on the help of people like you. Every contribution, no matter if it’s big or small, supports independent journalism and sustains our future.