Rozalyn Anderson Explains Caloric Restriction
At the University of Wisconsin-Madison, Dr. Rozalyn Anderson is studying one of the oldest-known and yet most powerful anti-aging interventions: caloric restriction (CR). Back in 1935, CR helped launch the entire longevity field when a pioneering study by Clive McCay and his colleagues at Cornell University demonstrated that CR without malnutrition significantly extends the lifespan of laboratory rats.
Almost 90 years later, scientists still study CR, and Rozalyn is at the forefront of this research. The golden standard of animal models is non-human primates, but lifespan studies in them last decades. Rozalyn is leading one of the very few studies of CR in monkeys, which began in 1989. Finally, we have lifespan data and a trove of other information that Rozalyn has presented at several recent conferences. We talked to Rozalyn about her fascination with CR and aging and the profound insights her study had produced.
How did you end up working on the biology of aging?
I started my first foray into aging research in David Sinclair‘s lab at Harvard. I came over from Ireland after completing my PhD in yeast to work in David’s lab, which at the time was mostly using yeast models. He had been working on genome instability in yeast but at that time, he became interested in aging and caloric restriction (CR) in particular.
Because my training was as a biochemist, I was immediately interested in the metabolic component. It fascinated me that you could study aging in yeast. We used to talk about “the awesome power of yeast genetics.” Using these tools, we uncovered a role for metabolism in delaying aging by CR.
This is how I got started in CR and the metabolism of aging. Toward the end of my post-doc, I discovered, quite by happenstance, that there were individuals studying mice on CR. That sparked my interest, so I moved to Wisconsin to work with Rick Weindruch. That was terrific, but then I discovered there were monkeys on CR, which led me to take an appointment with the Wisconsin National Primate Research Center, again with Rick Weindruch as my mentor.
As a scientific discipline, aging is fascinating. Aging animals aren’t broken – they’re just different. I try to stay away from the oversimplified idea that if something’s up with aging, we should bring it down, or if it’s down, we should bring it up. What we see with aging are often small changes from middle age to later age to advanced age. They’re not overt changes, just subtle alterations. I think this idea that things are altered rather than simply inhibited or activated is closer to the truth.
Another fascinating aspect is the heterogeneity of aging. Take inbred mice, for example. They’re genetically identical clones, yet in a lifespan study, you see a survival curve – some die sooner, some later. Even siblings or littermates in the same study can age very differently.
Instead of treating this heterogeneity as a problem to control for, we see it as a trait of aging. We’re doing quite a bit of work trying to understand this process, finding correlates among age-related changes and trying to trace back to individual events that might trigger the variation we see at advanced age. Each tissue has its job, each cell has its function, each zone has its control nodes, and they’re all massively integrated.
Let’s dive deeper into your area of research. Caloric restriction is among the most powerful anti-aging interventions we know.
It’s obviously something that delays aging when implemented correctly – we know different strains respond differently, sex is a factor, and diet composition matters, but you can extend longevity, not just survival, in animals on CR.
So, how does that work? What does it tell us about aging? You delay disease onset, reduce comorbidities, and extend survival time. What’s happening there that makes the pace of aging different in CR animals?
For me, it always comes back to metabolism. I believe all of life is about energy – metabolism and organization of energy, communication of energetic status, and decisions about where that energy is invested – it’s the ordering of energy that gives us life.
That resonates a lot with the perhaps simplified idea that it all comes down to the choice between growth and maintenance and that CR switches the organism toward maintenance. To what extent is this correct?
I think that’s absolutely it. We see metabolism and growth working as a tag team – not opposing each other but balanced with each other. One distinction I’d make is that when people talk about growth, they often think of things getting bigger. In fact, most of the time, it’s about growth signaling.
Growth signaling is a response to the availability of nutrients and energy so you can build and create. In adults, most cells are post-mitotic – they’re not dividing, which is good: if left unchecked, we’d be the size of a metro city bus by age 15. The mechanisms that regulate growth are also involved in how cells respond to things independent of increasing size, whether it’s an insult, a stimulus, or an inhibitory cue. Importantly, they work hand in hand with metabolism because executing any task requires available energy.
I think that’s the biggest missing piece in what we teach students now – the cost of being alive, the metabolic cost, the energetic cost. I remind students, and sometimes, it hits them like a revelation: we are precisely what we eat. Our entire body is synthesized based on what we’ve ingested. It’s amazing when you think about it.
If you’re a new parent nursing a child, you see how they grow based on what you provide before they transition to ingesting food. After that, for all of us, literally all the cells we replace, all the processes we maintain, all the experiences and tasks we execute – we do it using food as building blocks and as fuel.
A person’s body is most interesting for what it does, not what it looks like. When you think about what the body can do – growth and development through adulthood, producing offspring, responding to different environmental cues, healing itself, adjusting – it’s amazing.
What exactly does CR do to the organism? What are your main takeaways from these decades-long studies?
I think what happens with CR is that reduced nutrient availability stimulates a program involving increased efficiency and curtailed recruitment of growth signaling pathways. Growth signaling is dampened, and I believe the reduced immune decline and lower inflammatory tone we see are direct results of that growth signaling component.
People think of insulin as the diabetes hormone, but insulin is fundamentally a growth signal. When you have nutrients and energy, it’s time to make and store things. We’re so focused on insulin’s role in diabetes that its actual physiological role can be overlooked. When you have dysregulated growth signaling, you’ll have problems with any kind of adaptive response that requires coordination.
There’s an effect, a response, and a resolution of that response – all requiring tight coordination of energetic and signaling components. We think of this as homeostasis and resilience: the ability to respond and come back. These processes get leaky with age, and I think CR’s finer balance of improved efficiency and dampened growth helps prevent this dysregulation.
What is the role of fasting in CR?
It’s one of CR’s main features. What happens during fasting is a fuel switch – this is Biochemistry 101. When the body has no nutrients coming in, you get what’s called glucose sparing. The liver’s job is to use fat as a fuel source and deplete glycogen to give glucose to everyone else. Any tissue able to switch to lipid use will do so, preserving available stored glucose for cells and tissues that preferentially use glucose. As fasting extends, you get more gluconeogenesis, which is deriving glucose from other carbon sources.
Glycogen is like a big warehouse of glucose units that can be liberated. It’s periodic – if you’re fasting, you liberate it; if not, you won’t. When fed, you store it. When those glycogen levels get low, you ramp up gluconeogenesis, using amino acids or the glycerol component of triglycerides as the carbon source. These feed into biochemistry pathways to produce glucose.
During fasting, the idea is to share and spare glucose. If you’re the liver, you share it; everyone else agrees not to use glucose unless absolutely necessary – like being chased by a bear – and instead uses lipids. Lipids are a denser fuel and are entirely dependent on mitochondrial function because to use them as fuel, you need respiration.
I think this lipid turnover component is one of CR’s most important features. In obesity, you see lipids accumulating not just in cells but outside them, expansion of adipocytes in unwanted places, and elevated circulating lipids. Lipids are quite toxic – they’re hydrophobic and sticky, you don’t want them floating around.
CR clears everything out efficiently. The fat (adipose) tissue in CR animals is different – generally lower mass, smaller adipocyte size. We can see it by MRI in our monkeys. We also see fewer signatures of inflammation in CR adipose tissue compared to age-matched controls.
Adipose tissue is an endocrine organ, sending signals to regulate metabolism in other tissues. We’re particularly interested in a protein called adiponectin. It comes from adipose tissue and tells other tissues to use fat as a fuel source. Taking that clue from CR, where adiponectin levels are elevated, we started treating animals with a drug that mimics adiponectin to change their metabolism. In males, we can preserve physical function – they can run longer, faster, stronger when given this drug because it’s similar to CR.
Interestingly, adiponectin uses some of the same mechanisms as exercise – the kinase AMPK and the transcriptional coactivator PGC1 alpha. There’s an area of overlap in fuel use between exercise and CR. They’re not identical, but they share features. This explains why both exercise and CR produce health benefits, but with exercise, your growth signaling stays at full tilt, while with CR, it’s not. That’s why exercise improves health but not longevity, while CR does both.
Let’s go back for a moment. Can you give me some background on CR research on non-human primates? There were two big studies, the NIA study, and the UW study, and you’re continuing with the original UW study, correct?
That’s right. Our first paper, which showed that CR was effective in improving survival, came out in 2009. We published a follow-up later because some animals were still alive at the time of that first publication. We had MRI imaging showing differences in gray matter volume preservation in CR animals, and that was too significant to hold back until the lifespan component of the study was completed,
There had been earlier publications on things like sarcopenia and metabolic health, but we needed enough animals to pass on and reach sufficient age to discuss survival. In 2009, we had significant differences in age-related survival but not all-cause mortality because our numbers were small. By 2014, we had significant differences in both age-related and all-cause survival, plus differences in age-related conditions between controls and CR animals.
The NIH team, currently led by my friends Julie Mattison and Rafael de Cabo, published their study in 2012. Here at UW Madison, it’s currently Ricki Colman and me. Before, all of us were Don Ingram and George Roth at NIH, Rick Weinrauch, and Joe Kemnitz here at UW. The UW Madison study started in ’89, and while all our animals are gone now, I think they may still have a couple at NIA.
NIA didn’t seem to see the same effects we did, which created some controversy. Our groups got together to write a manuscript using data from both studies – something quite unusual. Julie and I even did a comedy sketch, giving talks together and poking fun at each other’s studies.
Looking at all the data together, one thing is absolutely clear: animals that eat less and weigh less live longer. The NIH had different cohorts, including very early onset CR, which in retrospect, might not be ideal for primates. In monkeys, very early onset probably has benefits outweighed by detrimental effects, but when CR begins in adulthood, things look good. Their old-onset cohort, starting at 20 years, included some of the oldest animals ever recorded in captivity, and those animals looked similar to our CR animals.
There’s a widespread perception in the longevity field that the UW group wasn’t receiving a very good diet, and CR simply minimized the deleterious effects of that diet, which led to the observed difference in lifespan.
That story was such a red herring! Let me tell you why. First, even though our control animals were pudgy – not slim and trim – they were only slightly overweight compared to the Primate Aging Database. The crucial point is that our CR animals got the exact same diet – they just ate less of it, were healthier, and lived longer. So, the diet itself doesn’t explain the differences we see.
The control animals were fed what we’d call an approximation of ad libitum, but their food was removed in the late afternoon. Both groups were effectively on time-restricted feeding with no food overnight. Our control animals completely align with the lifespan curve for monkeys in the US, sitting exactly on the line. Our median survival matched what everyone else in the monkey research world sees. They weren’t anomalous.
The diet issue came up because the formulations were different – purified diet at UW, naturally sourced at NIA. UW chose a purified diet to know exactly what was in it and avoid seasonal variation. Neither approach is better – they’re just different.
Rafa (de Cabo) invited me to join him in a study where he took both monkey diets – Wisconsin and NIA – and fed them to mice. His team gave ad libitum monkey diet to mice, and because of slight differences in density, they did a swap to pair-feed so animals got exactly the same calories. A separate group was put on CR using one or the other diet.
The results? Animals fed ad libitum lived exactly the same whether on a Wisconsin or NIA diet. The pair-fed animals lived the same as each other again, independent of diet, and the CR animals lived the longest of all, with no difference between Wisconsin and NIA diets. That was definitive proof that diet wasn’t the primary driver of differences between studies.
An interesting finding emerged – the pair-fed animals got their food in one meal, ate it within hours, and had no food until the next day. They were effectively time-restricted eating, unintentionally. They lived longer than ad libitum mice despite having the same amount of food. Studies since then have shown the fasting component contributes to lifespan extension with CR: the maximum benefit comes from fasting plus calorie reduction, but you can get some benefits just from fasting.
There’s not a lot of clarity on the effect size of time-restricted feeding, but you’re saying it does help?
Time-restricted feeding is a reasonable paradigm. When you look at all the evidence from caloric restriction, fasting, time-restricted feeding, and alternate-day eating across species – from yeast to flies to worms to mice to monkeys to people – it’s compelling. The fasting component is hugely beneficial.
One challenge – not that I’d tell anyone what to do – is the food people eat without realizing it. Snacks, especially in the evening, when you decide to have something nice, and before you know it, half the pack is gone.
There is some anecdotal evidence that time-restricted feeding might interfere with exercise. Interestingly, your CR monkeys at later ages remained fitter and had more muscle mass.
That’s right, we saw that effect. The idea of CR in opposition to exercise is interesting. It’s not difficult to see that exercise increases energy demand, and so it comes down to energy balance – you have to fuel the body to do what it needs to do. Look at master athletes or Olympians: they eat vast quantities of food to support enormous energetic output. The energy requirement for something like the pommel horse is mind-blowing – the strength, the training. That energetic demand must be met.
If you’re demanding energy through exercise while imposing energetic restriction, the system is at odds – you’re not delivering what the body needs for what you’re asking it to do. There are interesting data from the first phase of CALERIE, the NIH human caloric restriction study. The Pennington team compared a group of individuals on 25% calorie reduction with another group where a 12% reduction in calories was combined with a 12% increase in energetic demand. There were overlaps and similarities, but these two interventions were not the same. For a typical person with a normal life, the key might be some exercise and moderate eating rather than CR per se.
In terms of general health, it seems clear that metabolic fitness is crucial, and I’d separate that from body composition. Body composition usually correlates with metabolic fitness in population studies, but metabolic fitness is what’s important. Take diabetes: many people with diabetes are overweight or obese, but far from all overweight people have diabetes. The key difference is metabolic fitness. When you’re metabolically compromised, you’re open to chronic diseases.
Personally, I think the CR paradigm as a lifestyle is unappealing. From a scientific point of view, I think CR’s best value is in the insights it delivers about the biology of aging and sustaining health into older age.
Another interesting finding concerned the differences between visceral and subcutaneous fat. It’s a platitude that visceral fat is the “unhealthy” one, but you have shown how exactly it exerts its bad effects.
Adipose tissue is crucial, and lipids are important beyond just being fuel. All organelles are lipid membrane-bound; the cell has a lipid membrane, and receptors sit in lipid membranes. In many neurodegenerative diseases, we see imbalances in lipids or issues with how they’re used – as stores, structural components, or signaling molecules. We see subtle differences at the molecular level between subcutaneous and visceral adipose depots; metabolism pathways are enriched in the subcutaneous, and immune and inflammatory pathways are enriched in the visceral.
These tissues also respond differently to CR, which is likely to be highly relevant to humans. Adipose tissues are the major reservoir for lipids; they are released to be used as fuel and play a role structurally and as signaling molecules. When we look at the molecular level, the parallels between humans and monkeys are striking – how adipose tissue looks, subcutaneous versus visceral, matches what we see in humans, as does the response to CR.
When you run lipidomics in monkey plasma or other tissues, you see thousands of lipids, and we’ve only annotated and defined a small fraction. Exciting developments are emerging with spatial lipidomics. I saw a wonderful talk by Kristin O’Connell, who is based in the Jackson labs, showing spatial lipidomics in the brain – they can identify brain regions simply by lipid profiles. The brain is second only to adipose tissue in fat content. Differences in lipids across regions of the brain would have huge implications for neural growth, synaptic activity, and remodeling of neural networks.
We have compelling data from our monkeys through MRI, looking at gray matter volume and white matter integrity. We can see both age and CR effects. In specific regions of the brain, gray matter volume tracks with insulin sensitivity, and white matter integrity shows interesting connections to circulating cholesterol and adiponectin. Our PET imaging examining glucose uptake also shows connections to insulin sensitivity. In all these measures, there’s a link to peripheral metabolic status. What happens from the neck down completely influences what happens in the brain. I bet that the lipid story is going to be fascinating and extremely important for brain aging and cognition.
We touched briefly on CR mimetics, like adiponectin. Do you believe CR-mimicking drugs are feasible and can change how people age?
All exploration is valuable. The beauty of drug interventions is that you can examine changes in old animals over different time frames, immediate to long term, and then remove the drug to look for lasting effects. While there are plenty of molecules targeting specific pathways, right now, the tools we have align more with the hallmarks of the aging idea than the CR mimetic concept.
Take rapamycin: I’m involved in the trial of rapamycin in the Dog Aging Project. Evidence suggests that low-dose intermittent rapamycin is beneficial for healthy aging, but it’s not a CR mimetic – it’s more about growth suppression.
That said, you can recapitulate some CR aspects through growth suppression, similar to what we see in genetic mutant long-lived dwarf mice. Reduced growth signaling correlates with a more youthful immune system and less inflammation. Other approaches target senescence directly through things like SASP inhibitors, focusing on cytokine release or senescent cell pathways that are important in chronic inflammation.
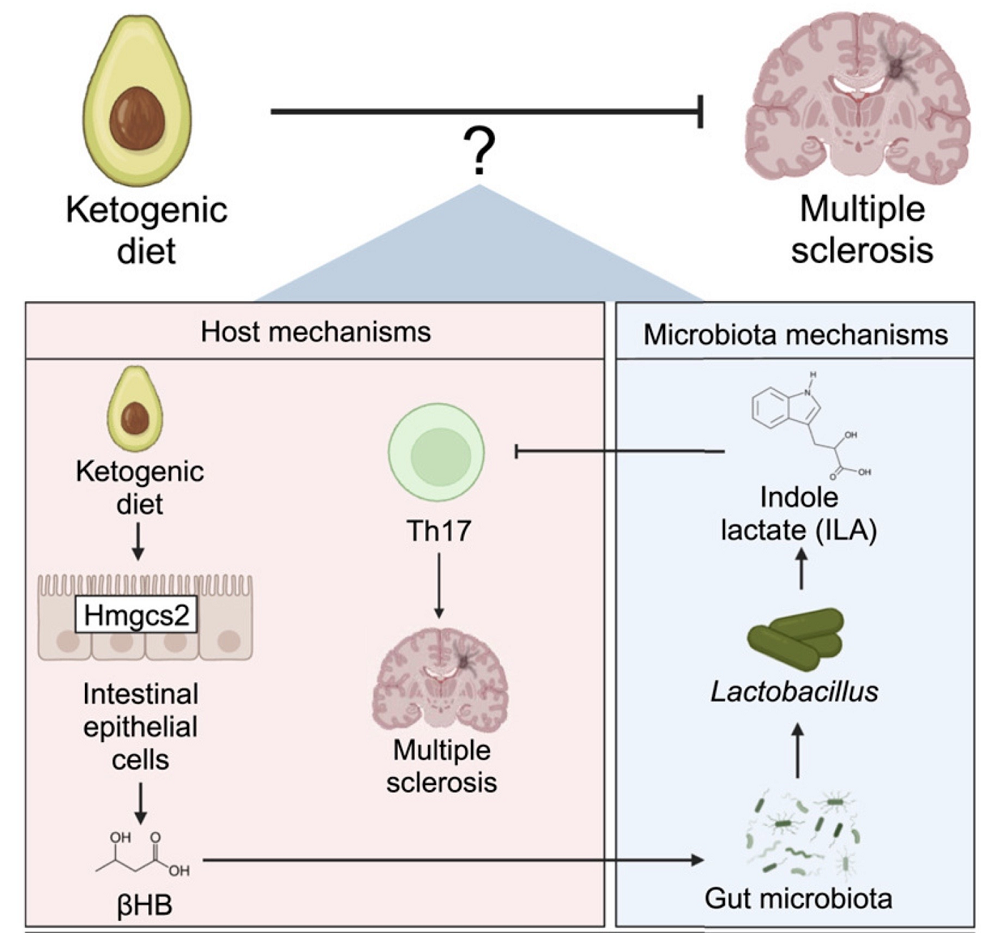
Metformin is closer to a CR mimetic, but it’s mainly effective in metabolically compromised animals, not healthy ones. The ketogenic diet is another interesting approach, acting as a fasting mimetic by recreating what happens during fasting.
What’s next for you after this extensive study?
NIH/NIA have been terrific in their support of this long-term big data monkey study. We’re still generating and analyzing the data. We’re collaborating with computer scientists, mathematicians, and bioinformaticians to build programs for data integration. There’s no established pipeline for this sort of thing – we’re blazing new trails in data analysis. It’s incredibly exciting.
Next year, we hope to publish findings on aging trajectories and inflection points specific to metabolites and lipids, developing biomarkers, and adding complexity. We have several studies on adipose tissue and brain in progress, with future plans for liver and skeletal muscle.
Thanks to funding from the Simons Foundation, we’ve maintained our brain research using the tissues from our Monkey Aging and CR study. One of the next things I’d love to examine is lipid tracers in the brain; it would be very cool to explore white matter integrity and neural network activity. We’re also engaged in studies of the effect of CR on neurovascular coupling and neural networks with live imaging capabilities, but those studies are only in mice. I am hoping to investigate how the brain takes out the garbage through a specialized lymph system.
One of my current interests is cells as communities. When you grow primary cells in isolation – neurons, astrocytes, hepatocytes – they do perform functions but not exactly as they would in a community. I’m fascinated by how cells communicate and support each other through information and metabolite delivery.
This represents the real frontier in aging biology – expanding from reductive research, which remains necessary, to understanding how everything works together. New technologies allow us to examine things spatially, study organoids in three dimensions, and observe cells growing together. The interactions between cells touching each other are different from cells merely sharing media and different still from isolated cells.