The authors of a recent study published in Aging Cell tested 21 groups of medication used by the elderly and reported that some of them impact aging biomarkers [1].
Repurposing existing drugs to fight aging
The search for drugs that slow aging includes finding new compounds and repurposing already-known drugs. Animal studies have suggested that drugs used for cardiovascular problems, diabetes, and urinary disorders can be potentially repurposed for anti-aging purposes [2]. However, studies in humans have been inconclusive [3, 4, 5].
Biomarkers of aging
The authors of a new study used data from three Swedish longitudinal studies to address the effects of the 21 most commonly used groups of medications on the speed of aging. The data was collected between 1986 and 2014 and included people who were 65.5 to 82.8 years old at the first in-person assessment. Participants were followed up for around nine years.
The authors believe that combining data from three studies strengthened their statistical analysis. Additionally, there were many individuals over 80 years old, a group that is commonly underrepresented in smaller studies.
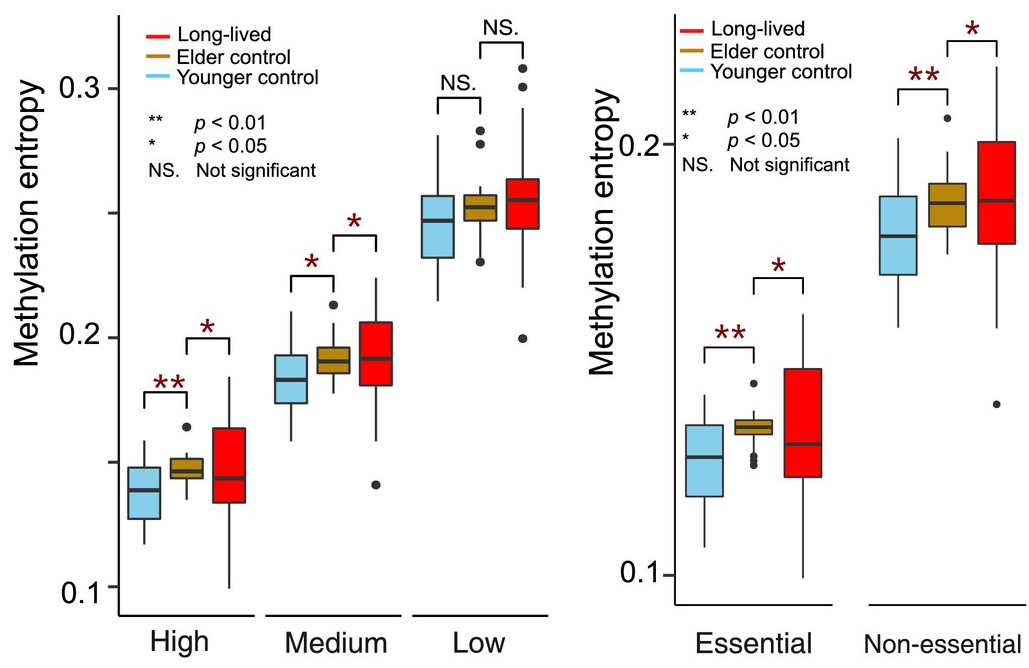
To measure the speed of aging, the authors used known biomarkers of physical decline with age: the functional aging index (FAI), an index of cognitive function (COG), and the frailty index (FI). The FAI quantified functioning, specifically sensory functioning, lung function, gait, and grip strength, with a higher score indicating worse performance. The COG is comprised of various cognitive tests to reflect general cognitive abilities. The FI is “the sum of the number of deficits a person has divided by the total number of deficits present in the index” [6]. Examples of such deficits are diseases or disabilities.
Common medications and aging biomarkers
As expected, as the age of study participants increased, the FAI and FI also increased while the COG declined.
Following modeling and statistical analysis, the researchers found a few significant associations. First, two specific groups, adrenergics and lipid-modifying agents, were associated with improved cognitive functions. Second, drugs that belong to selective calcium channel blockers with mainly vascular effects (dihydropyridines) were associated with an improved functional aging index. However, in the initial analysis, the researchers didn’t observe any benefits regarding the frailty index.
The authors compared their results to previous research on the topic. They elaborate that mixed results came from previous research on an association between selective calcium channel blockers, which are mainly used to treat hypertension, and improved FAI values. Some of those studies lacked proper control groups, which made interpreting the results difficult [7, 8, 9, 10].
The current scientific literature also lacks clarity regarding statins [11]. However, the authors observed that their conclusions are in line with the observational studies linking statin use to decreasing cognitive impairment or dementia risk. This was not the case for all the drugs tested [5, 12].
The authors hypothesize a possible mechanism through which lipid metabolism is linked to cognitive functions in the elderly. They stress the importance of lipids for brain function and the dysregulation of lipid metabolism observed in diseases such as Alzheimer’s, which results in cognitive decline. They hypothesize that statins might have anti-inflammatory and antioxidant effects and aid in regulating lipid metabolism.
There is less clarity and data regarding the connection between adrenergics and cognitive function. This drug group includes drugs dedicated to asthma, chronic obstructive pulmonary disease, or other respiratory conditions. The scientific literature suggests lactate metabolism [13] and mitochondrial dysfunction improvements [14] as possible mechanisms of action. However, it needs to be explored in more depth.
Sex-dependent differences
The initial analysis concluded that none of the medications affected frailty. However, the secondary analysis pointed to sex-dependent differences. Angiotensin receptor blockers contributed to improvement in FI in men. The authors point out that they cannot offer much explanation regarding the mechanism of action, as frailty is not well described in the scientific literature.
Instead, the authors elaborate on the importance of taking into account sex-specific effects when performing aging research. This is crucial due to the differences observed in aging patterns in men and women such as telomere lengths, epigenetic age, and immunosenescence. Men and women also differ regarding such biomarkers as physical strength [15].
Women also have “different pharmacokinetics (e.g., lower pH gastric fluid and lower basal metabolic rates), pharmacodynamics (e.g., lower renal clearance), adverse drug reactions compared to men, and different prescribing patterns” [16, 17, 18].
Our results contribute to previous discussions on aging as a potential target for drug discovery in addition to disease-based drug development. Adrenergics/inhalants, lipid-modifying agents/plain, and CCB may have an effect outside of their original indication, preserving an individual’s functional independence through improvements in FAI and COG. However, it is yet to be discovered their effects on individuals without the diseases the drugs are prescribed for, proper dosage, and duration of treatment. Investments in aging as a pharmacological intervention target could prevent adverse aging outcomes, e.g., neurodegenerative diseases, and reduce future high healthcare costs.
We would like to ask you a small favor. We are a non-profit foundation, and unlike some other organizations, we have no shareholders and no products to sell you. All our news and educational content is free for everyone to read, but it does mean that we rely on the help of people like you. Every contribution, no matter if it’s big or small, supports independent journalism and sustains our future.
Literature
[1] Lopes De Oliveira, T., Tang, B., Bai, G., Sjölander, A., Jylhävä, J., Finkel, D., Pedersen, N. L., Hassing, L. B., Reynolds, C. A., Karlsson, I. K., & Hägg, S. (2024). Effects from medications on functional biomarkers of aging in three longitudinal studies of aging in Sweden. Aging cell, e14132. Advance online publication.
[2] Barardo, D., Thornton, D., Thoppil, H., Walsh, M., Sharifi, S., Ferreira, S., Anžič, A., Fernandes, M., Monteiro, P., Grum, T., Cordeiro, R., De-Souza, E. A., Budovsky, A., Araujo, N., Gruber, J., Petrascheck, M., Fraifeld, V. E., Zhavoronkov, A., Moskalev, A., & de Magalhães, J. P. (2017). The DrugAge database of aging-related drugs. Aging cell, 16(3), 594–597.
[3] DeLoach, T., & Beall, J. (2018). Diuretics: A possible keystone in upholding cognitive health. The mental health clinician, 8(1), 33–40.
[4] Espinoza, S. E., Jiwani, R., Wang, J., & Wang, C. P. (2019). Review of Interventions for the Frailty Syndrome and the Role of Metformin as a Potential Pharmacologic Agent for Frailty Prevention. Clinical therapeutics, 41(3), 376–386.
[5] Zhu, X. C., Dai, W. Z., & Ma, T. (2018). Overview the effect of statin therapy on dementia risk, cognitive changes and its pathologic change: a systematic review and meta-analysis. Annals of translational medicine, 6(22), 435.
[6] Rockwood, K., & Mitnitski, A. (2007). Frailty in relation to the accumulation of deficits. The journals of gerontology. Series A, Biological sciences and medical sciences, 62(7), 722–727.
[7] Agostini, J. V., Tinetti, M. E., Han, L., Peduzzi, P., Foody, J. M., & Concato, J. (2007). Association between antihypertensive medication use and non-cardiovascular outcomes in older men. Journal of general internal medicine, 22(12), 1661–1667.
[8] Baptista, L. C., Amorim, A. P., Valente-Dos-Santos, J., Machado-Rodrigues, A. M., Veríssimo, M. T., & Martins, R. A. (2018). Functional status improves in hypertensive older adults: the long-term effects of antihypertensive therapy combined with multicomponent exercise intervention. Aging clinical and experimental research, 30(12), 1483–1495.
[9] Vaz Fragoso, C. A., & McAvay, G. J. (2020). Antihypertensive medications and physical function in older persons. Experimental gerontology, 138, 111009.
[10] Simon, C. B., Lee-McMullen, B., Phelan, D., Gilkes, J., Carter, C. S., & Buford, T. W. (2015). The renin-angiotensin system and prevention of age-related functional decline: where are we now?Age (Dordrecht, Netherlands), 37(1), 9753.
[11] Alsubaie, N., Al-Kuraishy, H. M., Al-Gareeb, A. I., Alharbi, B., De Waard, M., Sabatier, J. M., Saad, H. M., & Batiha, G. E. (2022). Statins Use in Alzheimer Disease: Bane or Boon from Frantic Search and Narrative Review. Brain sciences, 12(10), 1290.
[12] Adhikari, A., Tripathy, S., Chuzi, S., Peterson, J., & Stone, N. J. (2021). Association between statin use and cognitive function: A systematic review of randomized clinical trials and observational studies. Journal of clinical lipidology, 15(1), 22–32.e12.
[13] Dong, J. H., Wang, Y. J., Cui, M., Wang, X. J., Zheng, W. S., Ma, M. L., Yang, F., He, D. F., Hu, Q. X., Zhang, D. L., Ning, S. L., Liu, C. H., Wang, C., Wang, Y., Li, X. Y., Yi, F., Lin, A., Kahsai, A. W., Cahill, T. J., 3rd, Chen, Z. Y., … Sun, J. P. (2017). Adaptive Activation of a Stress Response Pathway Improves Learning and Memory Through Gs and β-Arrestin-1-Regulated Lactate Metabolism. Biological psychiatry, 81(8), 654–670.
[14] Chai, G. S., Wu, J. J., Gong, J., Zhou, J. L., Jiang, Z. Q., Yi, H. Y., Gu, Y., Huang, H. H., Yao, Z. Y., Zhang, Y. Q., Zhao, P., & Nie, Y. J. (2022). Activation of β2-adrenergic Receptor Ameliorates Amyloid-β-induced Mitophagy Defects and Tau Pathology in Mice. Neuroscience, 505, 34–50.
[15] Hägg, S., & Jylhävä, J. (2021). Sex differences in biological aging with a focus on human studies. eLife, 10, e63425.
[16] Skoog, J., Midlöv, P., Borgquist, L., Sundquist, J., & Halling, A. (2014). Can gender difference in prescription drug use be explained by gender-related morbidity?: a study on a Swedish population during 2006. BMC public health, 14, 329.
[17] Soldin, O. P., & Mattison, D. R. (2009). Sex differences in pharmacokinetics and pharmacodynamics. Clinical pharmacokinetics, 48(3), 143–157.
[18] Zucker, I., & Prendergast, B. J. (2020). Sex differences in pharmacokinetics predict adverse drug reactions in women. Biology of sex differences, 11(1), 32.