VitaDAO Backs Research into Chronic Oral Disease
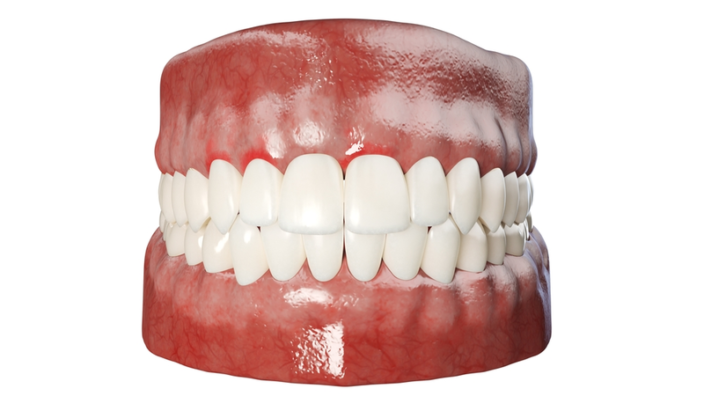
Periodontal disease affects more than 47% of adults aged 30 and over. For people over 65 years of age, that number rises to over 70%, making periodontitis one of the most commonly observed age-related illnesses.
Jonathan An’s lab seeks to research inflammation-targeting compounds that can help treat periodontal disease and reduce its negative impact on human longevity. Recently, VitaDAO, a biotech DAO funding early-stage research projects, voted to fund An’s project to the sum of $300,000 via an IP-NFT.
Research focused on gum health
Led by Dr. Jonathan An, Assistant Professor at the University of Washington, Dr. Matt Kaeberlein, Professor at the University of Washington, and Dr. Simon Johnson, Assistant Professor at the University of Washington, this periodontal disease research project aims to discover a geroscience-based treatment for age-related periodontitis.
Current therapies in the field of periodontal disease, such as scaling and deep cleaning, involve treating the symptoms of the disease rather than the underlying causes of the illness. Although periodontitis occurs in more than 70% of the population over the age of 65, little research has been done to specifically target the disease.
Jonathan An’s team proposes a novel approach that places the low-grade inflammation associated with both periodontitis and aging at the center of the lab’s research and seeks to test and record a series of compounds to treat such inflammation.
How is periodontitis research connected to longevity?
The underlying factor of low-grade inflammation in the absence of infection has long been noted in longevity science. Known as inflammaging, it is commonly observed not only in periodontal disease but also in other age-related illnesses, such as Alzheimer’s, heart disease, and diabetes. Dr. An’s team supposes that by targeting such inflammation, the onset and worsening of periodontal disease could be prevented, and there could be an additional positive impact on overall human healthspan.
By testing small molecule inhibitors of the PI3K/NFkB/mTOR pathway, the research team aims to establish a novel therapy for periodontal disease. As a positive control, the researchers plan to use rapamycin, which has supposed oral rejuvenation effects when used in mice. Drawing from this research, An’s team believes that these small molecules could ameliorate the inflammation that leads to periodontal disease or even the disease itself.
What is the role of VitaDAO?
In April 2022, 99.87% of VitaDAO voted in favor of funding Dr. An’s research with $300,000 (USD). The funding will be delivered under the DAO’s innovative IP-NFT format, which covers various elements of the project, including animal ordering and facility costs, the research team, inflammatory panels and antibodies, lab consumables and drug costs, microCT costs, and personnel wages.
VitaDAO believes that the lab’s geroscience-based approach could have a potential positive impact on inflammaging with wider-reaching impacts in the longevity field, such as possible discoveries about other targets in the PI3K/NFkB/mTOR pathway. In spite of the lab’s inexperience in entrepreneurial ventures, VitaDAO has confidence in the project’s feasibility.
Backing the project via an IP-NFT, the DAO believes a number of therapeutics could result from the research, including localized oral cavity treatments, such as compound-based toothpaste, drect delivery solutions to periodontal pockets, and compound trays, such as whitening tray solutions.
Although this project is still in its early stages, if successful, it may lead to further research down the line and additional spin-off projects that are closely related to the longevity field.
Summary
Receiving a 99.87% favorable vote, Dr. Jonathan An’s team was awarded $300,000 to fund its novel periodontitis research project that seeks to reduce inflammaging. VitaDAO believes such geroscience-based treatments will have a positive impact not only on oral health but also on longevity.