If humans ever reach an average lifespan of well over 100 years, what is going to happen? Are we going to be bored with such long lives? “Well,” says Prof. Brian Kennedy of the National University of Singapore, “If you ask me: ‘Do I want to have cancer at 75? Do I want have Alzheimer’s disease at 85? Or do I want to be bored at 110?’ I know which one I’m going to take.”
It’s hard to argue with that. Finding a new hobby to fend off boredom at age 110 is by far a better problem to have than having to look for your lost marbles at age 85, and Brian Kennedy—one of the top names in biogerontology—is working towards a world where healthy supercentenarians are commonplace.
Meet Prof. Kennedy
Up until 2016, Professor Kennedy was President and CEO of the Buck Institute for Research on Aging, a position to which he was appointed in 2010. While the Buck is still one of Brian’s academic affiliations, he currently serves as the Director of the Centre for Healthy Ageing and Professor of Biochemistry and Physiology at the National University of Singapore (NUS).
After earning a BA in Mathematics and Biochemistry, Molecular Biology, and Cellular Biology at Northwestern University, Kennedy was a doctoral student in Dr. Leonard Guarente’s lab at MIT, where he eventually got his PhD in biology. It was during this time that Kennedy’s interest for aging sparked and led to the discovery that sirtuins—a class of proteins affecting several cellular processes, aging included—influenced the longevity of yeast.
After his postdoctoral studies, which were centered on tumor suppression mechanisms, Brian left the Massachusetts General Hospital Cancer Center to become Assistant, and eventually Associate, Professor at the University of Washington. After Washington, his career as an aging researcher continued at the aforementioned Buck Institute for about six years, during which he also held the title of Visiting Professor in Aging Research at Guangdong Medical College in China. Today, in addition to his position at NUS, he’s also an Affiliate Professor at the University of Washington and an Adjunct Professor at the USC Davis School of Gerontology in Los Angeles, California.
His expertise in the field of aging research has earned Prof. Kennedy consultant and board member positions in several biotech and pharmaceutical organisations, such as Mount Tam Biotechnologies and SENS Research Foundation. He’s also co-Editor-in-Chief of the journal Aging Cell.
Prof. Kennedy’s research
Research at the Kennedy Lab, both in Singapore and back at the Buck, is focused on understanding the biology underlying the aging processes and finding ways to translate results into therapies applicable to humans that can delay, prevent and treat aging and the vast array of diseases that come with it.
Presently, Prof. Kennedy’s research projects focus primarily on the mTOR pathway to determine in which tissues it influences mammalian aging and how long-lasting any effects are.
The mechanistic target of rapamycin (mTOR) pathway is one of the four pathways that make up metabolism (IGF-1, mTOR, sirtuins, and AMP), and it has an influence on deregulated nutrient sensing, one of the reasons we age.
The mTOR pathway is composed of the mTORC1 and mTORC2 protein complexes. It senses amino acids and is associated with nutrient abundance. It is a kinase, meaning that it adds phosphates to molecules. mTOR is a master regulator of anabolic metabolism, the process of building new proteins and tissues.
A lower level of mTOR activity increases lifespan in model organisms, such as mice, yeast, worms, and flies. Though lower mTOR is not always beneficial beyond a certain point, very low levels can affect healing and insulin sensitivity and can cause cataracts and testicular cancer generation in mouse models.
The Kennedy Lab in Singapore studies aging in yeasts and nematodes as well, trying to figure out the interaction between different pathways that control aging. Prof. Kennedy’s other research interests include the genetics of diseases such as dilated cardiomyopathy, muscular dystrophy and Hutchinson-Gilford Progeria Syndrome, which resembles premature aging.
Advocating for healthier, longer lives
However, Prof. Kennedy isn’t just a prolific researcher with nearly 200 published papers. He’s also an outspoken supporter of healthy human lifespan extension and has shown his support in a number of ways and on multiple occasions. In 2016, he took part to the Intelligence Squared debate Lifespans are long enough alongside SENS Research Foundation’s CSO Dr. Aubrey de Grey, where both argued against the debate’s titular motion and won by a good margin.
Speaking of SRF, during Kennedy’s presidency, the Buck hosted the Rejuvenation Biotechnology Conference 2016 (RB2016) which was organized by the SENS Research Foundation. During the event, Kennedy gave a speech outlining the inadequacy of the current funding situation for aging research and the perils that our rapidly aging society will face during the first half of the 21st century if we don’t change our approach to treating age-related diseases. As he pointed out, we currently wait until individual diseases manifest and only then try to attack them one at a time, ignoring that aging is the common denominator driving them all. The result is that late in life, what we really do is not health care, but rather “sick care”, as all that is attained this way is keeping people in a state of debilitation for longer.
More recently, he has given a TEDx Talk as well, titled A Medical Revolution: Targeting aging directly, where he again stressed the importance of targeting aging to prevent not only human suffering but also the otherwise inevitable economic crisis fueled by spiraling late-life health care costs for an ever-growing proportion of people whose health conditions make them unable to contribute wealth anymore. That’s not all there is to it; according to Professor Kennedy, for the first time in human history, we’re close to being able to intervene against aging directly—and as our readership certainly knows, his conviction is shared by an increasing number of other biogerontologists. “We’re on the brink of a medical revolution,” he said in the talk.
To better understand the forthcoming medical revolution envisioned by Prof. Kennedy, we got in touch and asked him a few questions. This interview was taken at the Investing in Immortality conference, which was organized by Forbes Russia and non-profit organization Centaura (WayRay).
What, exactly, led you to study the biology of aging? Was it originally only scientific curiosity, or did you always have the goal of translating basic aging research into clinical applications?
It was totally scientific curiosity. When I got started as a graduate student, I wanted to take a project that was just exciting and answer a question that was totally unknown, and that was what causes aging. That’s been my focus when I started, but as I got more experience doing research in the field, and as I realized the challenge of the demographic population in so many people getting old, that I kind of modified my thinking. Now my primary focus is really on doing translation and extending healthspan, slowing aging.
Do you consider aging to be a disease or, at least, a co-morbid syndrome?
I think you can make an argument that it’s a disease, and you can also make an argument that it’s a risk factor for disease, but to me, fundamentally, it doesn’t matter. It’s the biggest driver of chronic diseases, loss of function late in life, and has a huge impact on life quality and health care costs. So we have to do something about aging, whatever you call it, and I don’t think it’s so important what we call it; it’s more important that we all agree that we have to slow down this process.
Do you think that the definition of aging as a disease called actually improve the regulatory situation with this status?
I think that it could certainly have a positive impact in a regulatory way, because if aging is a disease, then it’s much easier to develop therapies and get reimbursed for therapies, so I’m totally supportive of that effort. I think that, however, as I said in my talk, we don’t call cholesterol a disease, but we treat cholesterol because it’s a risk factor, so the FDA does approve interventions on targeted risk factors as well. I think we have to differentiate whether we’re discussing this from a conceptual point of view or from a regulatory point of view. Either way, we need the FDA to recognize the fact that aging is driving these other diseases that they care so much about, whether they want to call it a disease or recognize it as a validated risk factor. Either way, something has to happen so that we can develop interventions.
We sometimes hear people say that we don’t know enough about aging to do anything about it; however, others argue that we know enough now to start testing interventions and moving forward. Would you agree that we are at the point where we can start doing this?
I’m totally committed to the idea of testing candidate interventions in humans. I think we’re totally ready to do that; we have a range of safe interventions that we can test, so we have very low risk of doing harm, and the field will move forward dramatically if we can validate even one or two of these strategies. I believe exercise is more or less already validated, but what I’m talking about are some of the small molecule strategies and other kinds of interventions that are being developed. If we can validate that a couple of those work, I think it’ll have a huge positive impact on the field.
Targeting the aging processes directly is potentially the best way to prevent age-related diseases and the ultimate in preventative medicine. What do you think it will take for medicine to shift from the current infectious disease approach to age-related diseases to a preventative one?
I think it’s not an infectious disease approach, it’s really a treat disease approach that medicine has right now. The medical community does sick care; they don’t do much health care. Health care is prevention, and sick care is treating diseases, and we spend almost all of our research money and medical interventions’ cost on treating diseases. I think it’s pretty clear that that’s not the most effective way; if we can keep you from getting sick, it’s much better than letting you get sick and then keeping you alive. The challenge is how to change the medical community, the reimbursement system, insurance companies.
One of the reasons I’m in Singapore is that they have a public/private health care system, so everybody has a baseline public health care. Some people pay for more private health care as well, but the government pays a significant component of the health care costs for the individual, and that means the government is incentivized to keep people healthy. If we can develop interventional strategies and validate them in Singapore, we can go to the government and say “you don’t have to make money on the intervention.” We’re going to save a tremendous amount of money by keeping people healthy five or 10 years longer, and that’s really our goal.
If you look at the health care system in the U.S., it’s so screwed up with so many perverse incentives that it’s hard to figure out how you would even develop a drug that slows aging, and that that’s not an indictment on aging research, that’s an indictment on the health care system. I think places like Singapore, which publicly finance healthcare, are much better positioned to be the leaders in trying to develop aging interventions.
You were previously based at the Buck for a number of years and were an incredibly important figure there; what was your motivation to change gear and move country?
There wasn’t just one motivation, but I can answer the question in the following way. I wanted to go somewhere where we had to build into clinical studies which really tested interventions in humans, and that means I needed a research center that has good preclinical research, good basic science, but also hospital and clinical studies that are available, so the center we’re trying to build now is much more clinical in nature. I feel like that’s an important step because, as I said, we’ve developed a lot of ways to slow aging in animals, we need to validate that these things work in humans now, and I feel like Singapore is a good place to do it.
Singapore is projected to have a population made up of nearly 50% of senior citizens by 2050; what do you think will be the biggest challenge facing the elder care sector?
I think that we have to change the system. You can’t just build hospitals, because there are multiple challenges with that. First of all, you have a lot of sick people on a small island; it’s hard to treat all of them. There are not enough doctors and not enough hospitals; there are not enough caregivers to take care of older people. Perhaps most importantly, there are not enough younger workers to keep the economy going to pay for all the costs of the older people.
We have to change the paradigm. I don’t think there’s any solution on Singapore except keeping people healthy longer. We’re going to have to raise the retirement age. The people that are working later, they’re already doing that, and that’s not going to work unless those people are healthy and functional. We think we’re trying to provide an essential component of what Singapore and other countries like it need to get through this demographic crisis that’s happening in the next 30 or 40 years.
How receptive have you found the government and healthcare sector in Singapore to the idea of longer and healthier lives through the development of therapies that target the aging processes directly? How hard was it to convince them?
I think it’s still a process. We haven’t convinced everybody in the government; we have people that really understand and are supportive, and we have other people that we’re still talking to. The thing that excites me about the Singapore government is they think progressively. This is a party that’s been in power for a long time, it’s a democratic country, but the same party has won for many years. It’s probably justified because they’ve dramatically improved the life quality of the population in Singapore in the 1960s.
This was a relatively poor country with a lot of problems, and now it’s one of the richest countries in the world with very low corruption and a very good healthcare system. A lot of things have been accomplished, and the government thinks, “What can I do now to have a positive impact 10 years from now”, and that’s very hard to find in a government these days.
If you look at the U.S. government, everybody’s just worried about the next election cycle, and that’s true of a lot of other democratic governments as well. You have other kinds of governments that may have their own challenges, but if you can find someplace that’s really willing to spend money now that will only return on investment 10 years from now, I think you’ve found a place that has a lot of potential, and I think that’s the most promising thing about Singapore.
You are focusing on the mTOR pathway, part of the deregulated nutrient sensing hallmark of aging. What made you choose this particular pathway as the subject of your studies?
We didn’t choose mTOR, mTOR chose us. Essentially, what happened is that we were screening the simple organism yeast, where we can measure aging really quickly. We were just knocking out every gene one by one by one and finding out which genes lead to longer lifespan, and then we clustered those genes trying to figure out what pathways they’re in. The pathway that jumped out at us was the mTOR pathway.
We were particularly excited about that, because there is a drug, rapamycin, that can inhibit mTOR in mammals and humans even. So there was a clear path toward testing whether mTOR inhibition would have an impact on mammalian aging, and many, many labs have now shown that you can extend lifespan and slow aging, including some work from our lab in mouse models.
Now there’s studies going on in humans that are exciting. I think that it’s emerged now as one of the major pathways that affect aging, and it’s been fun to work on it for the last 10 years; the challenge is that we still don’t really know why reducing TOR activity leads to healthspan extension and lifespan extension, so there’s a lot of basic biology that needs to be done. I’m not planning on giving up on TOR anytime soon.
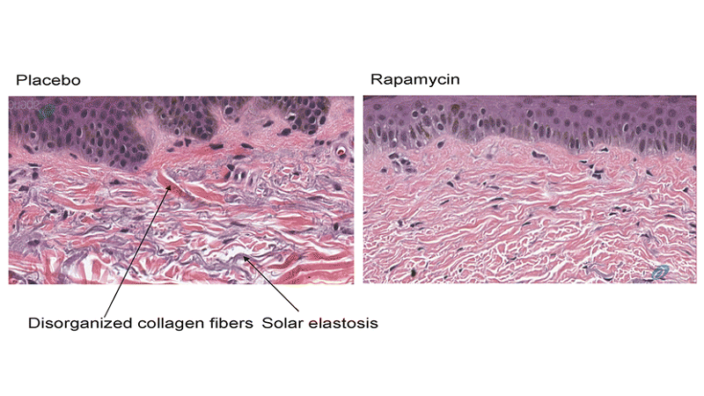
Rapamycin is the most commonly thought of mTOR inhibitor, but it can suppress the immune system and may have other harmful side effects. Are you investigating the so-called rapalogs as an alternative to rapamycin, and, if so, how do they compare?
There’s two components to this. The first is that there have been studies with current drugs like rapamycin and everolimus in healthy people, and if you dose effectively, you can dramatically reduce side effects. I think there’s potential even for the current generation of rapalogs to be effective.
Having said that, we’ve been working hard in our lab and through a couple of companies to try to develop new versions of rapamycin that have higher efficacy and lower side effects because rapamycin is very effective, but it does have side effects, and that narrows the therapeutic window in which you can give the drug. If we can either improve the efficacy or reduce the side effects, then we have a broader therapeutic window and we can have a better impact, so we’re excited about trying to make derivatives of rapamycin that work even better, but the first generation of drugs look promising on their own.
A number of people interested in longevity already try to reduce mTOR signaling via approaches such as fasting and caloric restriction; do you practice any of these things, and, if so, have you found a method that suits you best in particular?
Yeah, my lifestyle makes it a little bit difficult to control my diet that well because I’m traveling constantly. However, when I’m in one place, I try to do time-restricted feeding where I eat really just one big meal a day and then try to eat within a narrow window during the day. I think that approach tends to work for me well, but it’s hard for me to stay consistently on it because when you start switching time zones every week, it influences your diet. I also try to exercise and do some sort of endurance training and a little bit of resistance training.
Most importantly for me, I’ve been trying to work on stress levels, because, especially when I was CEO of the Buck, there were a lot of things going on. There’s always a problem somewhere in an institute that big; the Institute’s great, but every institute has its problems that you’re dealing with, so if you take all that home and you’re constantly worried about something, your stress levels get very high and that’s not very good, so I’ve been trying to differentiate the signals that generate stress that come in from how I respond to them. I think that that kind of mindfulness is probably beneficial too, so I’d say I’m not a lifestyle freak in terms of being healthy, but I try to do as much as I can to have a healthy lifestyle. Some of this things impact the mTOR pathway, and some of them impact other pathways.
You are also investigating alterations to nuclear lamins, which appear to influence epigenetics and thus gene expression. Progeria is perhaps the best-known example of where defective lamins cause accelerated aging, so do you personally consider progeria and regular aging closely linked?
I suspect that altered lamin function is one of the drivers of normal aging. I don’t think that’s been completely proven yet, but I think the bulk of the data suggests that’s true. The mutation that causes progeria is a dominant mutation, so it makes the protein do something new, and that causes toxicity. It’s very unclear whether that specific variant of the protein occurs in normal individuals or not. There’s some evidence for it, but it’s not strong.
However, lamins go through this proteolytic processing as they’re made, and so you make a large protein that gets clipped into a shorter protein. There’s evidence that that clipping could become defective with aging, and when you have the unclipped longer protein, it has some effects that are very similar to progerin. So we think that unprocessed lamin may be driving aspects of normal aging, and we’re trying to study that.
It still looks like they are closely linked.
I think that we sort of know this. It’s not called a progeria per se, it’s called a segmental progeria. What’s meant by that is that certain aspects of aging are accelerated in these kids and other aspects are not. For instance, they don’t have neurologic problems. They don’t get Alzheimer’s disease. They don’t have cognitive impairment. But they do have cardiovascular disease, particularly strokes, heart attacks, they have cachexia, they lose hair, their hair turns grey. Some aspects of aging are happening and others aren’t. I think that there are probably a number of disease conditions that are segmental in that way. In fact, I think a lot of diseases are linked to aging. It’s just that a lot of these diseases only affect a couple processes of aging, and progeria affects a number of processes of aging.
I’m asking you because a few years ago, I heard Claudio Franceschi saying that in his view, age-related diseases can even be considered as an accelerated aging of a particular system within the human body. So, in some people, some aspects, some systems age faster, and this is why we see age-related diseases manifest.
I agree with that. That’s what differentiates the outcome of one person aging from another person aging, and another way of saying that is personalized aging. We have to really begin to understand not just how we age the same but how we age differently to have the biggest impact down the road, I think.
Do you think that progeric strains of mice serve as useful models of human aging, or do you think, as some critics do, that they are not an accurate representation of real aging?
I think they represent an acceleration of some pathways of aging and not others, so they have value, but I don’t think it’s fair to say that you can learn everything about normal aging by studying any particular progeria model. I’ll give you an example, for instance, that we’ve been studying the mouse model for Hutchinson-Gilford progeria, the lamin mutation. In our hands, rapamycin does not extend the lifespan of that mouse. In normal mice, it does.
There’s a lot of evidence that affects normal aging, but in that particular context, it’s not improving things. Whereas, you know, if you enhance NAD levels with nicotinamide riboside, then we do see positive impacts on aging even though nicotinamide riboside has less of an effect in normal mice. That would suggest that maybe the sirtuin pathways affected in the progeria models, but the TOR pathway’s doing something different, so some aspects of ageing are accelerated and not others. So, the model’s useful, I just think that it becomes dangerous when you say that this recapitulates all of aging, because none of the models do.
Is there a question you never get asked by journalists that you would like us to ask you about your work?
Wow, that’s a hard one. I haven’t been stumped in a long time. I don’t know that I can point to any one question. I think that maybe what I would say is that I rarely get asked anymore what actually causes aging, and we discussed that today. I think that that’s the fundamental challenge in aging right now, as we know how to do interventions to slow aging, and we’re learning how to measure aging with biomarkers, but we still don’t know what causes aging. I think that the people that ask the right biologic questions to answer that are going to be very famous in this field.
Many people say that the hallmarks of aging are the causes.
Yeah, but I don’t think that gets the proximal causes, like you can say altered nutrient signaling, but the altered nutrient signaling is in response to something earlier. You can say DNA damage, but we don’t know how much DNA damage really contributes, and it’s not going to be zero, but it’s not going to be 100% either. Altered stem cell function with age, why, why? How much of inflammation that we see with aging is made by these senescent cells, and how much of it comes from other pathways? These are all open questions, so hallmarks of aging are good at pointing us in the right direction. I think there’s general consensus that most people believe these hallmarks are important, but how they interact with each other, and what are the proximal causes of aging, I still think are open questions.
We would like to ask you a small favor. We are a non-profit foundation, and unlike some other organizations, we have no shareholders and no products to sell you. All our news and educational content is free for everyone to read, but it does mean that we rely on the help of people like you. Every contribution, no matter if it’s big or small, supports independent journalism and sustains our future.



 We conducted a pair of conflicting interviews: one with Dr.
We conducted a pair of conflicting interviews: one with Dr. 
 This month’s interviews were of
This month’s interviews were of  We conducted two more interviews that month: one with demography expert
We conducted two more interviews that month: one with demography expert  The very first CRISPR trial on human beings was used as a therapy against cancer; it began with three people and grew to encompass more.
The very first CRISPR trial on human beings was used as a therapy against cancer; it began with three people and grew to encompass more. We interviewed Professor
We interviewed Professor