A Popular Senolytic Treatment Causes Brain Damage in Mice
- The effects are similar to multiple sclerosis.
- Administering dasatinib and quercetin to older mice causes their neurons to express less myelin and fewer outgrowths.
- This resembles the symptoms of multiple sclerosis.
A new study calls for caution in using the well-known senolytic treatment of dasatinib and quercetin (D+Q), showing that it causes damage in certain regions of the brain, similar to what is observed in multiple sclerosis [1].
Stem cell senescence prevents brain repair
Multiple sclerosis (MS) is a brain disorder in which the patient’s own immune system attacks oligodendrocytes: cells in the nervous system that provide a myelin coating for neurons, which is essential for their function and survival. MS is much more common in older patients, who are also more likely to have progressive disease and a worse response to treatment.
This has been linked to an increase in senescence among neural progenitor cells (NPCs) [2]. NPCs are stem cells that can repopulate lost oligodendrocytes and restore their function in the brain. In patients with MS, many NPCs are senescent, meaning that they’ve lost their ability to divide and instead remain in the tissue, promoting local inflammation. This observation has led the authors of a new study published in the journal PNAS to explore whether clearing away senescent cells may improve MS outcomes, with potential implications for other neurodegenerative diseases.
Effects on a healthy brain
To test this idea, the researchers administered the well-known senolytic combination of D+Q to aged mice. D+Q became popular after it was found to kill senescent cells in culture while generally sparing non-senescent cells [3]. It is considered the gold standard for senolytic interventions and has advanced to clinical trials for senescence-related conditions, including diseases of the lungs and kidneys, diabetes, and general age-related frailty, with promising results.
However, D+Q is not perfect. Both D and Q target molecules and molecular pathways that are not entirely unique to senescent cells, which runs the risk of off-target effects. Nevertheless, few studies have examined the effects of D+Q on a healthy brain, and this study was conducted to fill that gap.
D+Q stresses and reduces function in oligodendrocytes
The authors delivered D+Q orally three times a week on alternating weeks. In previous studies, similar protocols were found to extend the lives of mice.
One month after the start of the treatment, they collected the rostral corpus callosum (CC), a part of the brain connecting the left and right frontal lobes. The CC acts as a central wiring structure between the two hemispheres and balances the controls of higher cognitive functions. Neurons in the CC are organized into bundles that are wrapped in layers of myelin.
The CCs were analyzed by transmission electron microscopy (TEM) to measure myelination and compare it between treated and untreated mice. Surprisingly, D+Q treatment reduced myelination levels. The reduction was very modest but statistically significant. This was later confirmed in young animals, suggesting that the effect is age-independent.
Further analysis found that the treatment did not kill oligodendrocytes but altered their morphology, making them less complex and causing them to retract their outgrowths and reduce myelin deposition. This change occurred within 20 minutes of treatment onset.
To understand the underlying cause of this effect, the authors analyzed gene expression patterns in cells treated with D+Q. They found that cells that had received D+Q exhibited extensive endoplasmic reticulum stress, a condition in which newly produced proteins are not folded properly.
This led to the silencing of the machinery that normally controls myelin deposition. The injured oligodendrocytes still maintained myelin production and their cellular identity, but they were no longer able to deliver and organize myelin correctly, leaving the neurons exposed. In many ways, these changes are similar to those that occur during MS.
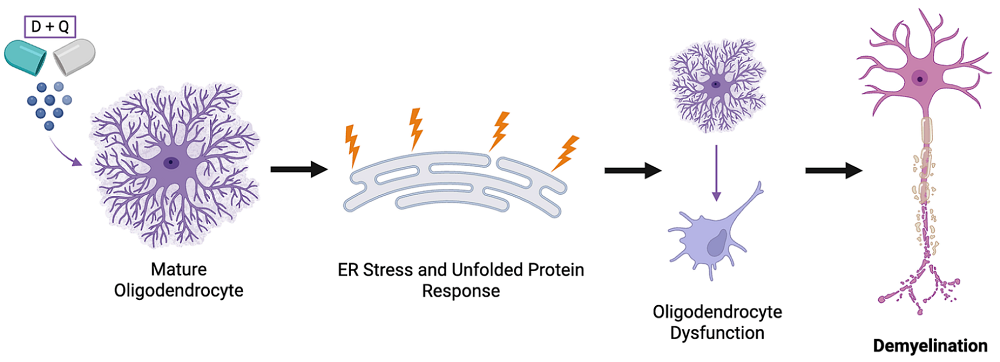
Key takeaways
For people who are interested in using senolytics to extend life and healthspan, this study serves as a warning that some treatments may have unintended and serious consequences. It’s a call for caution and for the discovery and development of more selective treatments.
For MS researchers, however, the study points to a surprising opportunity. The D+Q treatment affects oligodendrocytes in ways similar to those observed in MS, but the cells themselves remain viable. Hence, the changes they experience may be reversible, making D+Q a useful model to study that possibility.
Literature
[1] Lombardo, E. R., Pijewski, R. S., Lustig, J. T., Dhari, Z., Lahiri, A., Papile, L. E., … & Crocker, S. J. (2026). Senolytic treatment induces oligodendrocyte dysfunction and demyelination in the corpus callosum. Proceedings of the National Academy of Sciences, 123(12), e2524897123.
[2] Nicaise, A. M., Wagstaff, L. J., Willis, C. M., Paisie, C., Chandok, H., Robson, P., … & Crocker, S. J. (2019). Cellular senescence in progenitor cells contributes to diminished remyelination potential in progressive multiple sclerosis. Proceedings of the National Academy of Sciences, 116(18), 9030-9039.
[3] Zhu, Y. I., Tchkonia, T., Pirtskhalava, T., Gower, A. C., Ding, H., Giorgadze, N., … & Kirkland, J. L. (2015). The Achilles’ heel of senescent cells: from transcriptome to senolytic drugs. Aging cell, 14(4), 644-658.