Don’t let your birthday get you down and remind you that you are getting older; there are plenty of reasons to be cheerful about the future and your place in it, especially as science is now turning its attention to aging.
Another trip around the sun
So here I am again, another birthday just gone and another journey around the sun under my belt, so I thought I would do my customary musing about the future as I do every year.
For me, the idea of getting older does not bother me; what concerns me is the ill health and loss of independence that accompanies aging. It is absolutely irrefutable at this point that advancing age leads to developing the various diseases of old age to the point that one of them eventually kills you. No matter how well you live, no matter how carefully you diet and work out, sooner or later (considerably later if you exercise often), aging is going to catch up with you.
This year was actually a bit of a milestone for me as I have reached level 45, and while I wish I could stop earning experience points now and stay at this level, this is not an option; after all, nothing can stop the advance of time.
Okay, but what about stopping aging? Well, it turns out that this is unfortunately also unlikely to happen, yet.
I say yet, because as a journalist, I am keenly aware that many researchers are now engaged in research and unlocking the secrets behind aging and developing ways to allow us to get chronologically older without becoming biologically older. Your biological age is really the most important thing because it determines how aged your body really is; chronological age is just a number on your driver’s license.
So it is that my birthday finds me perfectly happy to grow chronologically older; I am just less keen on getting biologically older. That’s the trick: while it is not possible to stop advancing in chronological age, which is simply a measurement of how many times the world has orbited the sun since you were born, it is becoming increasingly clear that biological age is another matter entirely, and there is a real chance that science might do something about that.
Staying future positive
During my professional life, people frequently ask me how close we are to defeating aging. This is a perfectly understandable and fair question, of course; the problem with the question is that it’s also very hard to answer given how complex it really is.
A pretty big reason for this is because while aging is not too complex to understand, and indeed we will fully understand it sooner or later, there are a number of things that we need to tackle. It turns out there are at least nine reasons we age and possibly some other reasons that we don’t fully appreciate or even know about yet. This makes developing therapies to target these root causes very challenging, and there are many pitfalls and problems that can arise during research and development.
However, that does not mean that aging is too complex to understand for us to eventually bring it under medical control, which really seems to be just a question of time at this point. It’s no longer a matter of if we can do something about aging; it’s just a matter of how soon.
To help people to keep track of progress, we have created the Rejuvenation Roadmap, a database that charts promising therapies and how close they are to being available. Also, while I am always more than happy to talk about the progress happening in the field, I also urge people to explore the field themselves so that they can learn and evaluate for themselves rather than simply taking my word for it.
During my work, I speak to hundreds of researchers in the field as well as supporters of the research and members of the general public, who often know nothing about the field. I encounter a range of responses, including pessimism, which occurs surprisingly more often than I expect from people in the immediate and supposedly supportive community rather than the general public. In many cases, I find that the researchers are more upbeat about our chances of success than anyone else.
It is perfectly natural to be cautious about the unknown, but there comes a point when that caution can morph into unwarranted pessimism. We should, of course, fully acknowledge the challenge that defeating aging represents, but, at the same time, we should avoid being excessively negative given that there is plenty of reason to be future positive, which is why I remain so despite another year having passed.
Today, I am going to take a look at what I consider the most currently promising approach against aging: senolytics.
The future might be closer than you think
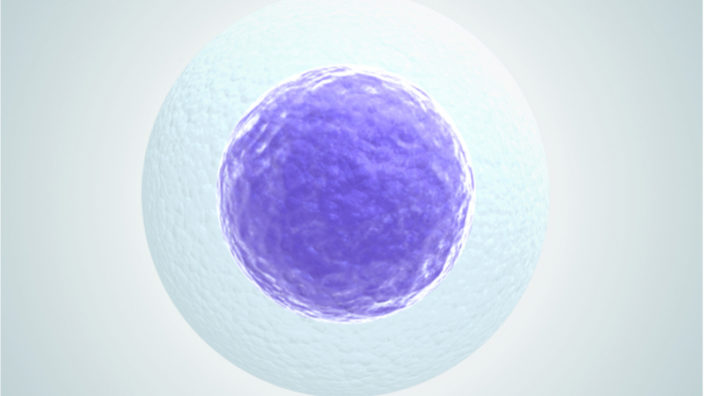
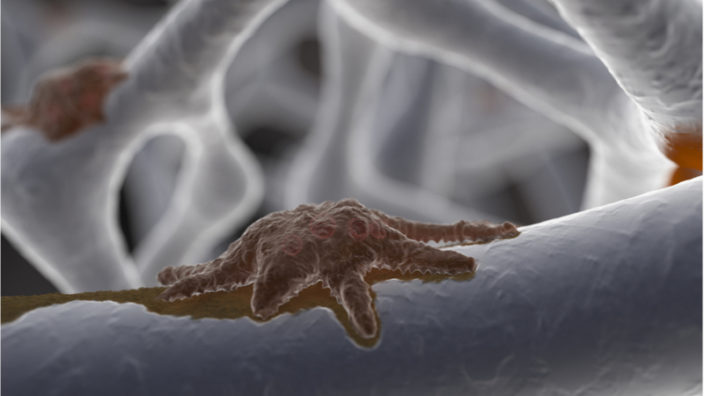
Senescent cells are aged or damaged cells that should destroy themselves via a process known as apoptosis but, for various reasons, do not do so; instead, they hang around, sending out inflammatory signals that harm nearby healthy cells, block effective tissue repair, and contribute to numerous age-related diseases. One proposed solution is to remove these problem cells by causing them to enter apoptosis, as originally intended, using senolytic drugs and therapies.
Senolytics are probably the most advanced of the therapies that directly address an aging process in order to prevent age-related disease and keep tissues and organs working more youthfully.
UNITY Biotechnology has been the leader of the pack since interest in developing senolytics burst into a frenzy of research a few years ago, and the company has been conducting human trials of its lead candidate drug (UBX0101) since earlier this year.
UBX0101 blocks the activity of the P53 pathway, which some senescent cells use to evade apoptosis and cling to life; by inhibiting this pathway, it causes these cells to self-destruct.
In February 2020, UNITY announced the launch of a Phase 2 study of UBX0101 in patients with moderate to severe osteoarthritis of the knee. This trial will evaluate three different doses (0.5 mg, 2 mg and 4 mg) of UBX0101.
Also, in March 2020, UNITY announced that it is were launching a Phase 1b study of UBX0101 in patients with moderate to severe osteoarthritis of the knee. This trial will explore the safety, tolerability and initial efficacy of a single 8.0 mg dose or multiple doses (two 4.0 mg doses separated by one month) of UBX0101.
We anticipate that the results of both of these human trials will be announced in the second half of 2020.
UNITY also has another candidate drug (UBX1967) closely behind; this drug targets the BCL2 pathway, another way senescent cells escape apoptosis, and it is slated to enter human trials for the treatment of age-related macular degeneration, diabetic macular edema, diabetic retinopathy, and glaucoma. UBX1967 is currently undergoing the investigational new drug (IND) application process, which is the first step in the drug review process by the U.S. Food and Drug Administration prior to launching human trials.
UNITY is not the only game in town when it comes to senolytics; Cleara Biotech is another biotech company working on this problem with a FOXO4-DRI peptide known as Proxofim. Proxofim was discovered by Dr. Peter de Keizer and has been in development since 2015 as a senolytic. In past studies, aged mice treated with Proxofim saw health benefits, including improved fitness, a glossier coat, and improved renal function.
However, the drug is not ready for human trials yet and is currently on its third generation of refinement. Cleara is now working hard to improve its potency, safety, and selectivity as part of its iPROX program to create an improved version. It is the company’s hope that the greatly refined and safer iPROX drug will allow translation to humans and the launch of clinical trials. Proxofim is likely a few years away from reaching human trials, but it is certainly something worth keeping an eye on as things develop.
Perhaps the most interesting company working on senolytics for me personally is SIWA Therapeutics, which is also working on senescent cell removal and has been busy developing 318H, a humanized monoclonal antibody. According to the company, 318H is being developed to slow or even reverse aging by removing harmful senescent cells but can also target cancer cells.
A few years ago, researchers at SIWA discovered that senescent and cancerous cells both have an advanced glycation end product (AGE) marker on their surfaces; this is due to both kinds of cells being oxidatively stressed and having abnormally high levels of glycolysis, which is known as the Warburg effect.
They then designed a monoclonal antibody specific to the AGE marker, which binds to the cells of aggressive cancers and senescent cells. They tested a mouse version of 318H in mice, and it removed senescent cells and promoted muscle regeneration. It also significantly reduced cancer metastasis in a model mouse of breast cancer.
If SIWA is successful with this immunotherapeutic approach to senescent cells and cancer, it would be an absolute game changer and allow for the effective treatment of cancer and a slew of age-related diseases associated with the accumulation of senescent cells.
There are a number of other interesting companies working on senolytic therapies including Oisín Biotechnologies, Senolytic Therapeutics, and Foxbio, to name a few; as time passes, others will almost certainly join them.
Based on the progress so far, it looks like senolytics are most likely to be the first true rejuvenation therapeutics in the sense that they directly target an aging process, and, in the next few years, we may see some of the first generation of these therapies arrive. When that day arrives, it has the potential to change how the world sees and treats aging, and that day will be a great day indeed. Stay future positive; we are getting closer to our goal!
We would like to ask you a small favor. We are a non-profit foundation, and unlike some other organizations, we have no shareholders and no products to sell you. All our news and educational content is free for everyone to read, but it does mean that we rely on the help of people like you. Every contribution, no matter if it’s big or small, supports independent journalism and sustains our future.